the obligate intracellular and nonculturable bacterial agents
- Rickettsiae spp
- Chlamydia spp
- Ehrlichia spp
- Coxiella burnetii
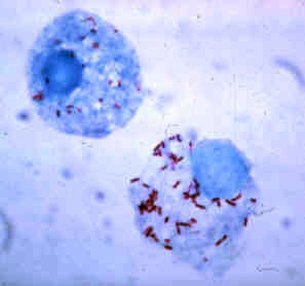
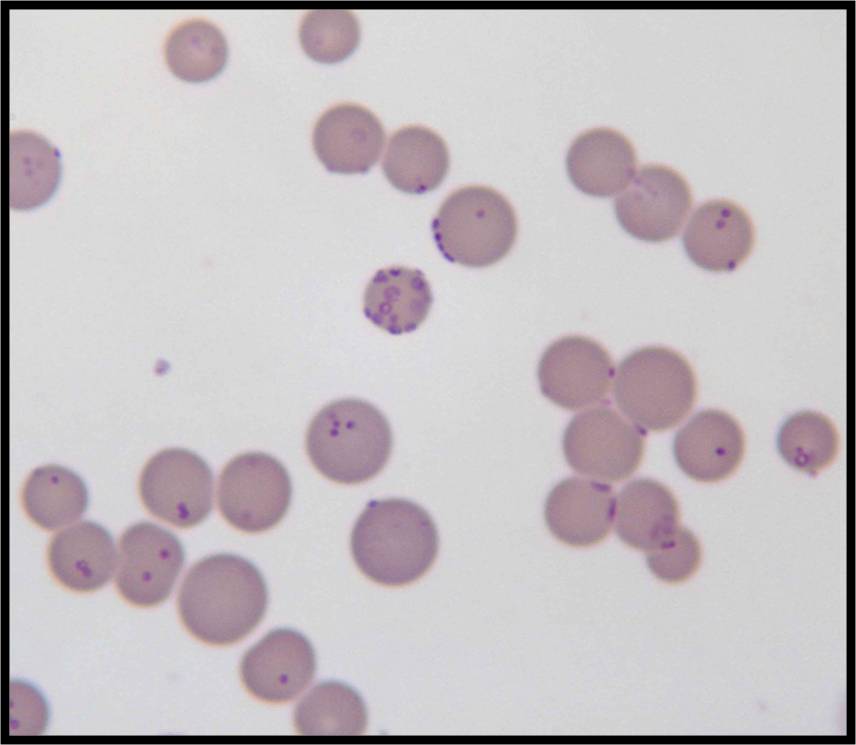
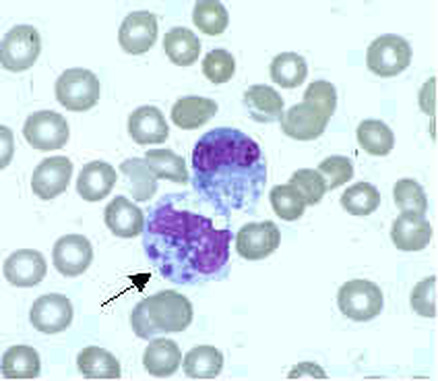
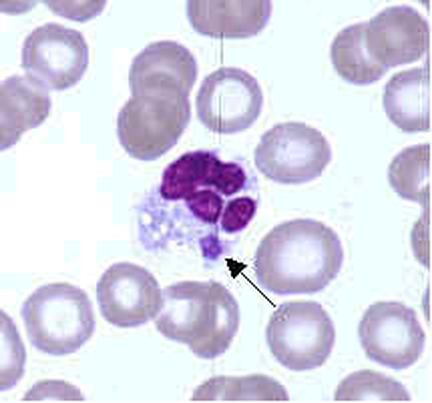
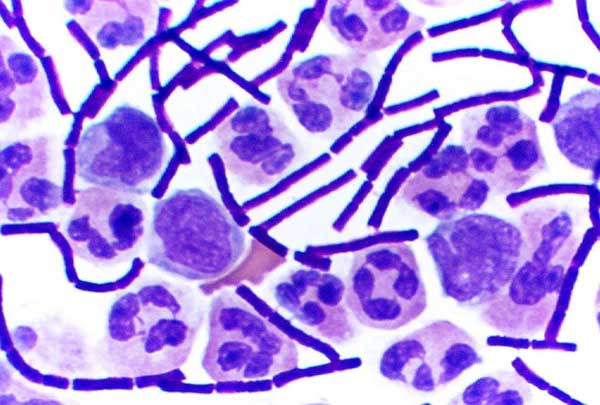
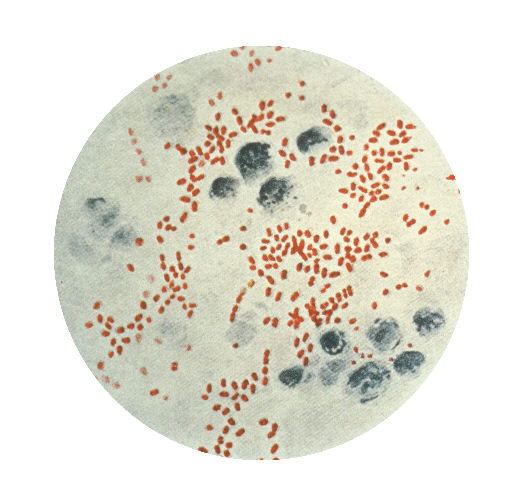
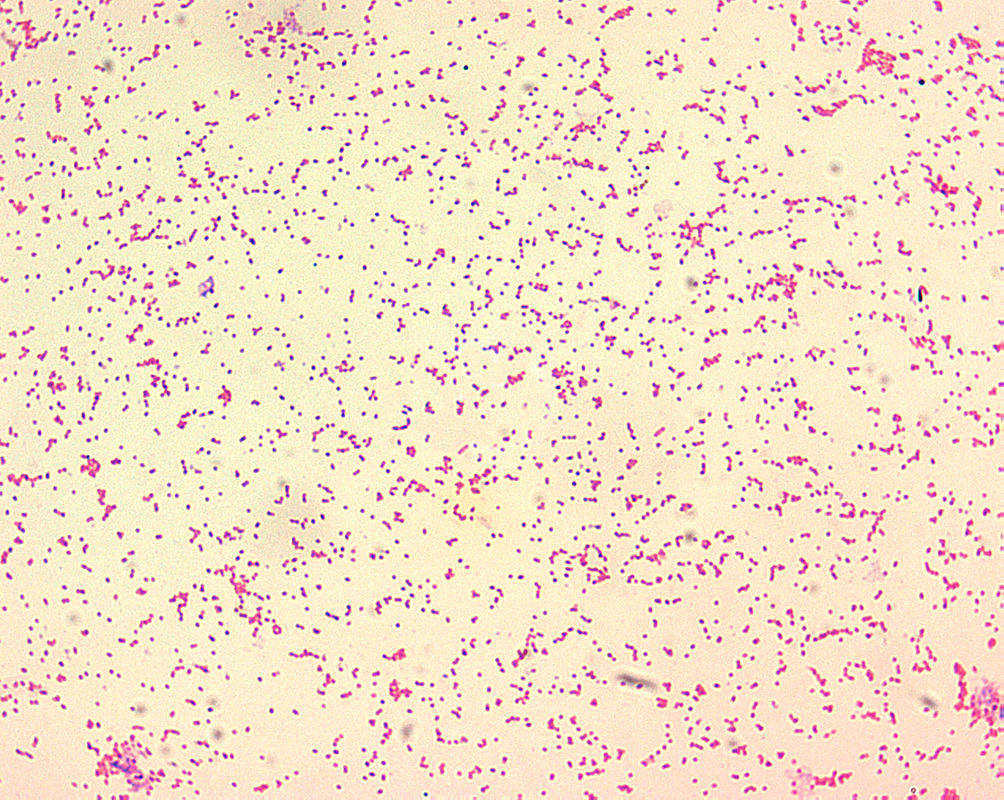
Rickettsiae
- R. prowazekii causes epidemic typhus, and was responsible for the deaths of many US soldiers due to typhus during World War II
- This is an obligate intracellular parasite that replicates inside endothelial cells of the reticuloendothelial system
- Aerobic, Gram-negative bacterium
- Carried by the feces of lice (human body lice)-Pediculus humanus
- The flying squirrel is the main reservoir
- The bacterium is surrounded by a protein microcapsular layer and a slime capsule
- Immunization tends to provide lifelong immunity, as does prior infection with the organism
- Rarely, may cause a latent infection which may reactivate years-to-decades later (Brill-Zinsser Disease)
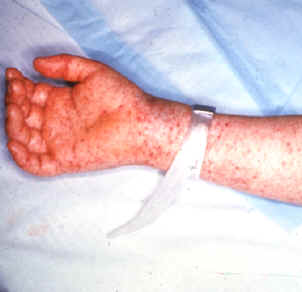
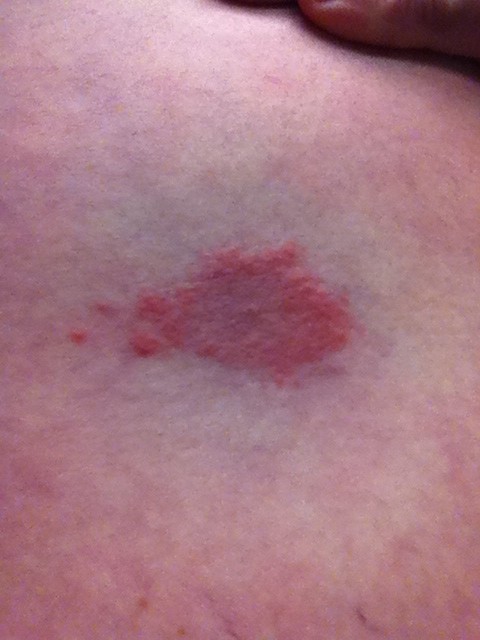
- Causes a maculopapular rash
- Rickettsiae bacteria are carried by chiggers, ticks, and fleas as well
- R. typhi causes murine typhus
- R. rickettsii is the causative agent of Rocky Mountain Spotted Tick Fever
- Causes fever, headache, muscle ache, and characteristic rash along with nausea, vomiting, loss of appetite, abdominal pain, joint pain, forgetfulness
- Carried by Dermacentor ticks
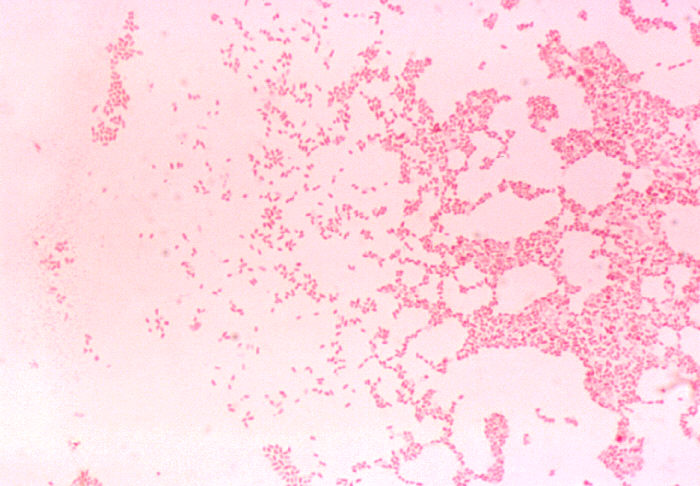
chlamydiae
Chlamydiae Spp:
-Obligate intracellular parasites (bacterial)
-Infectious Particle: Elementary Body
-Nonreplicating; Released when cells rupture
-Noninfectious Particle: Reticulate Body
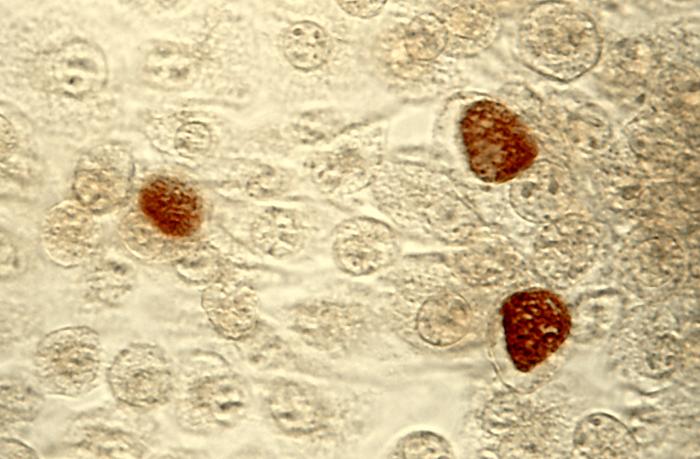
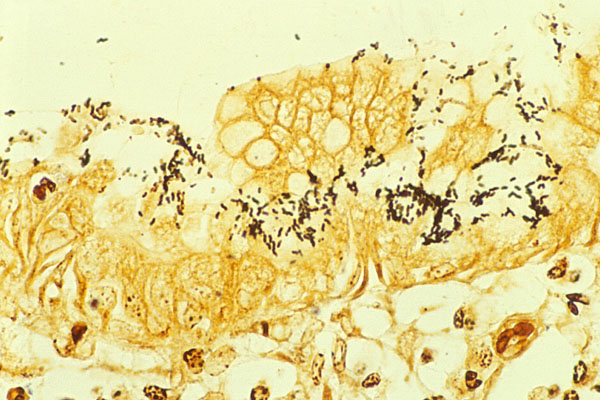
-Appear as brown inclusion bodies in the cell when stained with iodine
-Rigid cell wall
-Genome contains DNA chromosome and DNA plasmid
-Possess a heat-stable, genus-specific antigen that is part of the cell membrane lipopolysaccharide
-Reticulate body (intracellular growth and replication)
-Metabolically inert, infective form: elementary body (extracellular) resembling a Gram-negative bacillus without a peptidoglycan layer (round or pear shaped EB)
A. C. trachomatis
-STD (most common sexually transmitted bacterial pathogen)
-Major cause of Pelvic Inflammatory Disease (PID)
-Causative agent of urethritis, cervicitis, epididymitis
-Also causes conjunctivitis (ocular trachoma) and can lead to blindness
-Can be transmitted to the neonate from an infected mother during the birth delivery, and can cause neonatal pneumonia or inclusion conjunctivitis
-Can replicate well inside McCoy Cells and diagnosis is based on cytology, culture, direct detection of antigen or nucleic acid, and by performing serological testing
-Specimen is collected by a large endocervical swab or brush or urogenital swab
B. C. pneumoniae
-Community-acquired pneumonia
-Atypical pneumonia
-Bronchitis
-Pharyngitis
-Sinusitis
-A flu-like illness
-Mild-to-moderate illness in young adults or adolescents; Severe illness in elderly or respiratory-compromised patients
-Don’t stain well with Gram-stain
C. C. psittaci
-Respiratory psittacosis in humans
-Associated with close contact with infected birds (parrots, parakeets)
-Obligate intracellular parasites (bacterial)
-Infectious Particle: Elementary Body
-Nonreplicating; Released when cells rupture
-Noninfectious Particle: Reticulate Body
-Appear as brown inclusion bodies in the cell when stained with iodine
-Rigid cell wall
-Genome contains DNA chromosome and DNA plasmid
-Possess a heat-stable, genus-specific antigen that is part of the cell membrane lipopolysaccharide
-Reticulate body (intracellular growth and replication)
-Metabolically inert, infective form: elementary body (extracellular) resembling a Gram-negative bacillus without a peptidoglycan layer (round or pear shaped EB)
A. C. trachomatis
-STD (most common sexually transmitted bacterial pathogen)
-Major cause of Pelvic Inflammatory Disease (PID)
-Causative agent of urethritis, cervicitis, epididymitis
-Also causes conjunctivitis (ocular trachoma) and can lead to blindness
-Can be transmitted to the neonate from an infected mother during the birth delivery, and can cause neonatal pneumonia or inclusion conjunctivitis
-Can replicate well inside McCoy Cells and diagnosis is based on cytology, culture, direct detection of antigen or nucleic acid, and by performing serological testing
-Specimen is collected by a large endocervical swab or brush or urogenital swab
B. C. pneumoniae
-Community-acquired pneumonia
-Atypical pneumonia
-Bronchitis
-Pharyngitis
-Sinusitis
-A flu-like illness
-Mild-to-moderate illness in young adults or adolescents; Severe illness in elderly or respiratory-compromised patients
-Don’t stain well with Gram-stain
C. C. psittaci
-Respiratory psittacosis in humans
-Associated with close contact with infected birds (parrots, parakeets)
mycoplasma and ureaplasma: cell wall-deficient bacteria
- M. pneumoniae is the causative agent of atypical pneumonia, or walking pneumonia; Causes RBC agglutination (cold agglutinin disease)
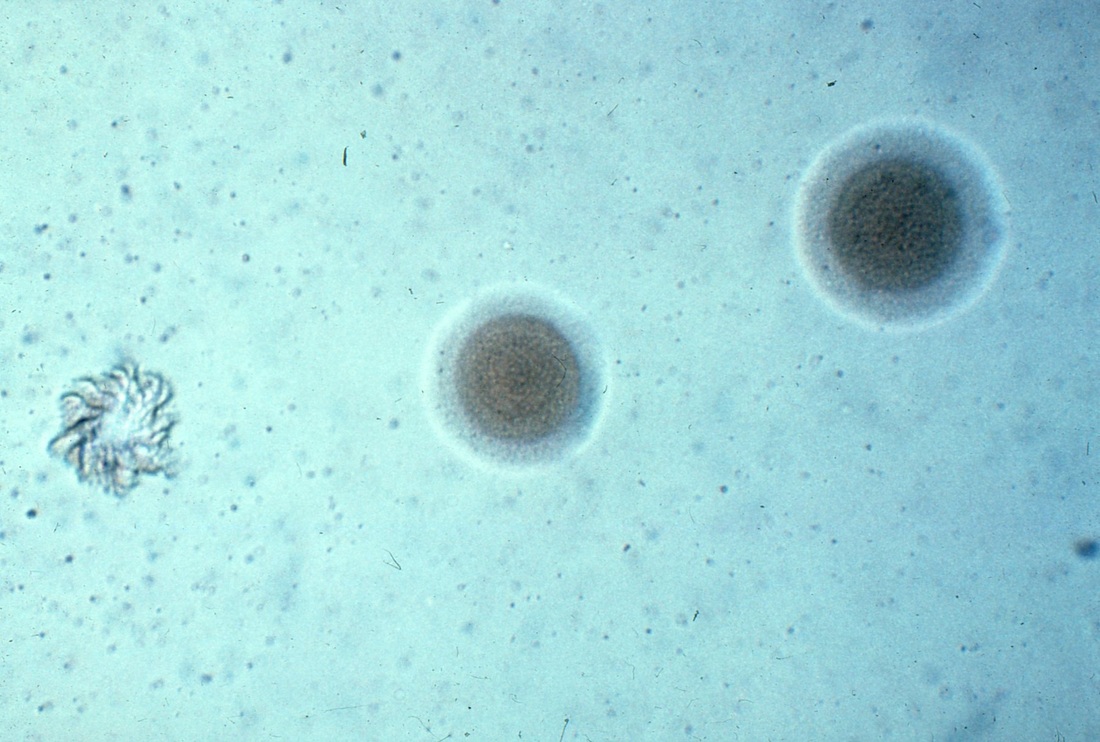
- Mycoplasmas are the smallest known free-living forms
- Lack a cell wall
- Referred to as "L-Forms"
- Have been recovered from the blood of patients treated with antibiotics that interfere with cell wall synthesis
- Part of the microbial flora of humans, mostly in the oropharynx, URT and genitourinary tract
- M. pneumoniae and M. hominis have been isolated from humans, and M. pneumoniae is associated with community-acquired pneumonia (walking pneumonia)
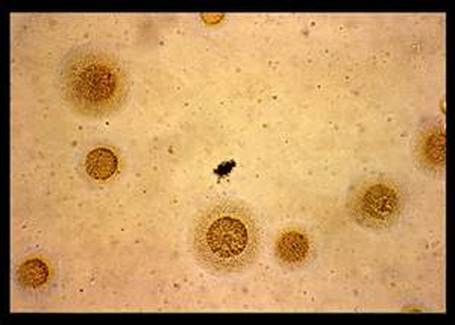
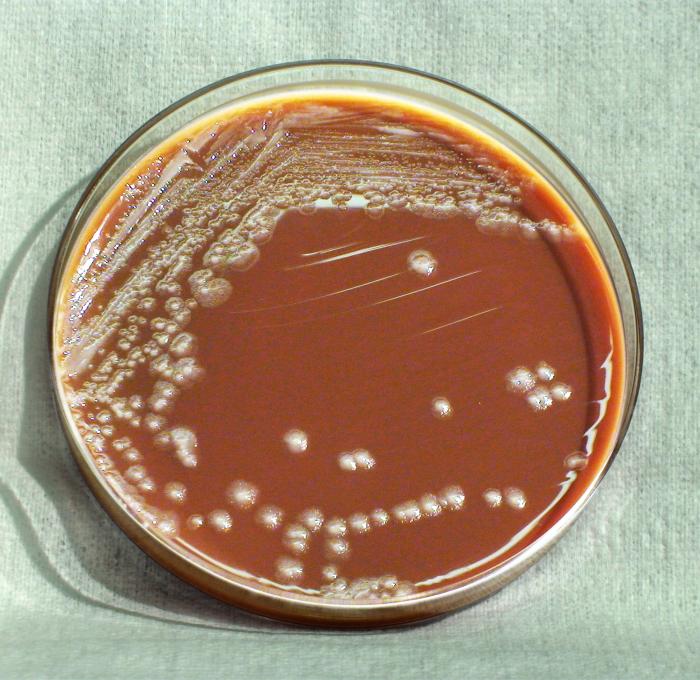
- Looks like "fried egg", a large, spherical, grainy yellow colony embedded in the agar with a thin, outer layer. Examine the surface of the agar under 40x magnification every 24-72 hours. These colonies are urease negative.
- M. hominis, on blood agar, produces nonhemolytic, pinpoint colonies that do not stain with Gram stain. They can be stained with acridine orange.
- Some Mycoplasma spp are associated with bacterial vaginosis, cervicitis, PID, infertility, stillbirth, preterm delivery, spontaneous abortion: M. genitalium
- Some Mycoplasma spp are associated with UTI: M. hominis
- Some Mycoplasma spp are associated with fetal respiratory distress syndrome, bronchopulmonary dysplasia, intraventricular hemorrhage in preterm infants
- Some Mycoplasma spp are associated with transformation of normal cells into cancerous ones: M. fermentans, M. genitalium, M. hyorhinis (colon, prostate and gastric cancers), M. penetrans and some are associated with lung and renal cancers
- Ureaplasma urealyticum is associated with UTI (rare), and M. hominis is rarely associated with UTI as well
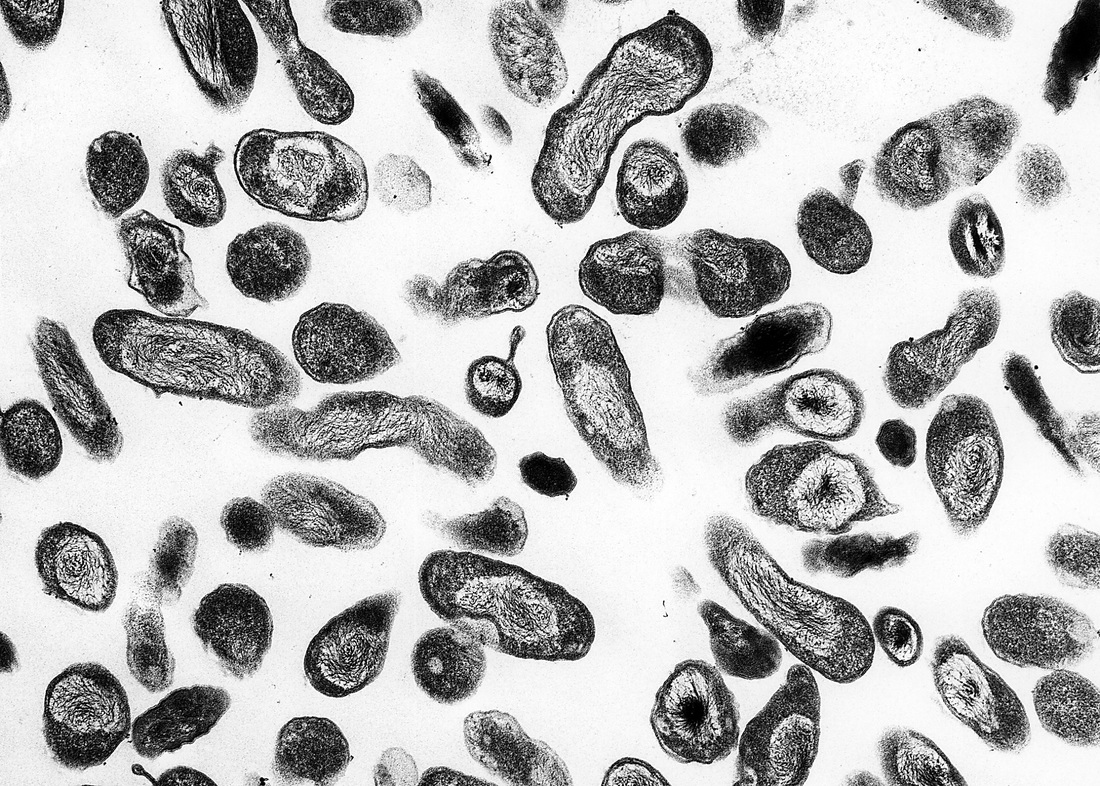
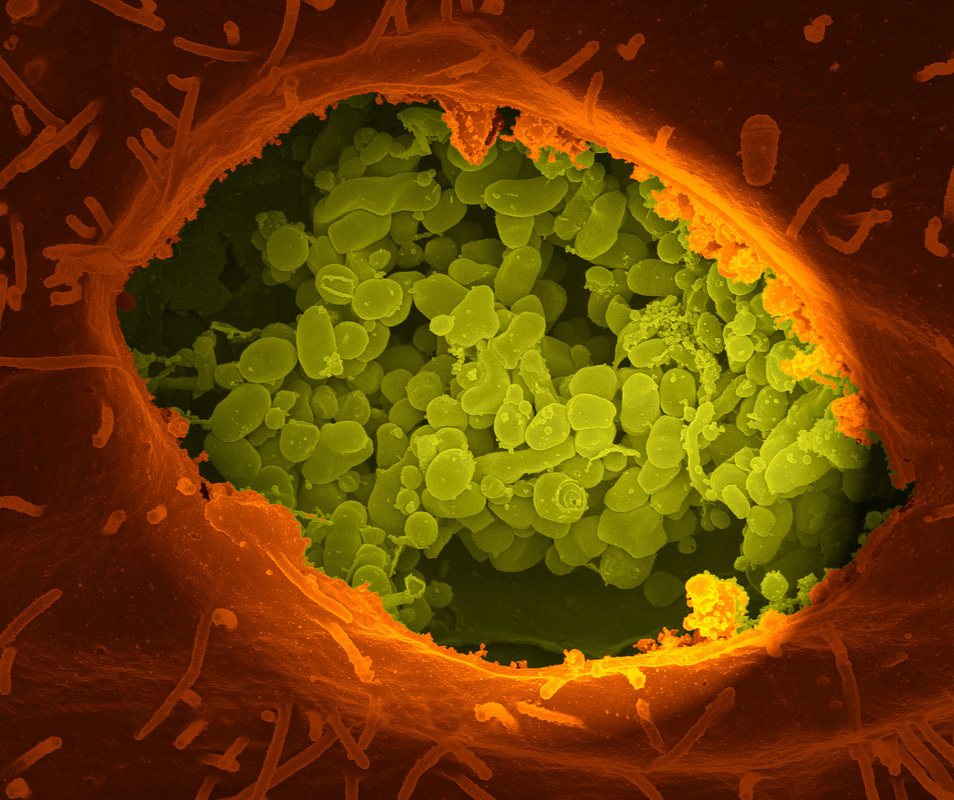
coxiella burnetii
- Causes Q-Fever
- Primarily affects the lung and grows only in the lung cells
- Smaller than Rickettsiae
- Resistant to many chemical and physical agents
- Obligate intracellular pathogen
- GN coccobacilli
- Reservoirs include cattle, sheep and goats
- Infection occurs via inhalation of contaminated aerosol particles
- Incubation period is 2 weeks to 1 month
- Symptoms include headache, fever, chills, myalgias, and may be acute or chronic. No rash develops.
- May be cultured and identified utilizing shell vial assays with human lung fibroblasts
- The most reliable serologic test for the diagnosis of Q Fever is the complement fixation test
- Infections are treated with tetracyclines
ehrlichia spp
- Causative agent of Ehrlichiosis, a tickborne illness
- E. chaffeensis is the main type and infects human monocytes and causes human monocytic ehrlichiosis after a tick bite
- E. phagocytophila and E. equi primarily infect neutrophils, causing human granulocytic ehrlichiosis after a tick bite
- Symptoms include fever, headache and rash
- Severity of illness ranges from mild-to-severe and the majority of patients infected with E. chaffeensis require hospitalization
- Approximately 2-3% of patients infected with E. chaffeensis die
- Immunohistology and PCR are used to diagnose infetions
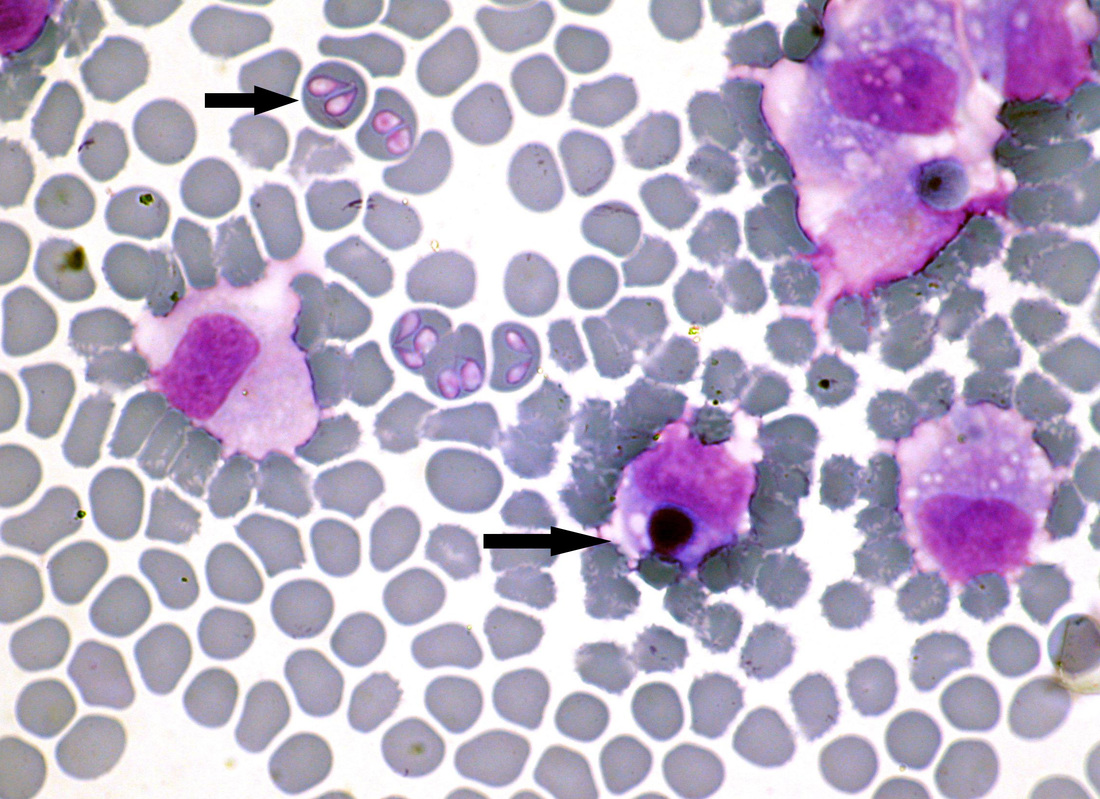
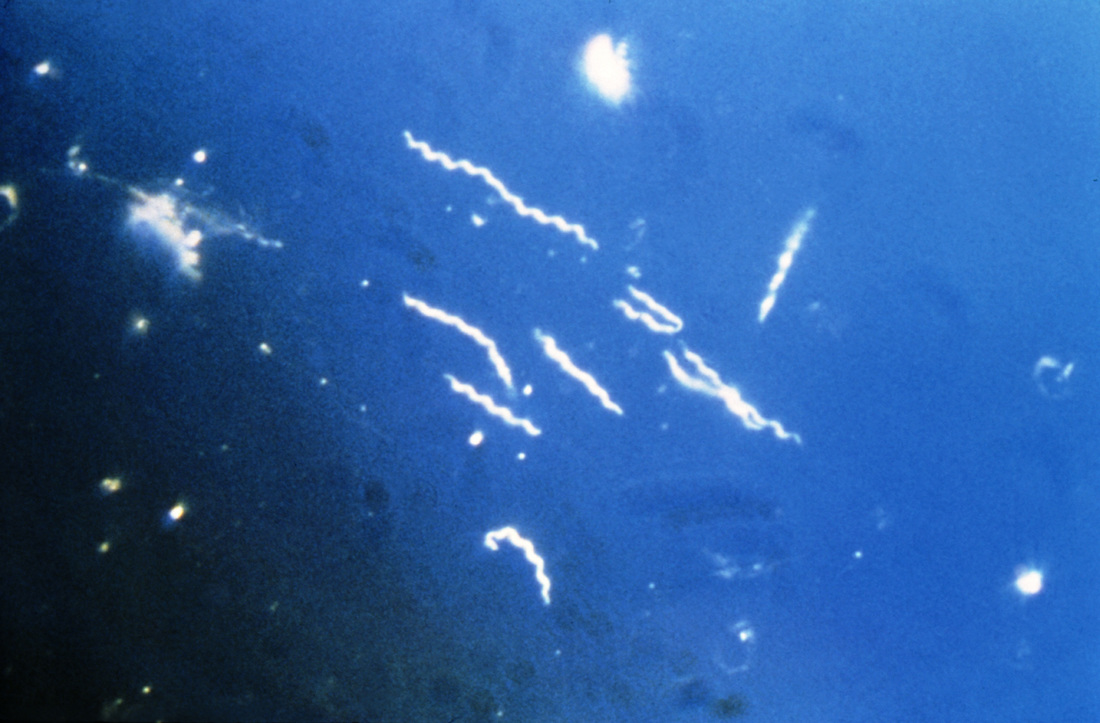
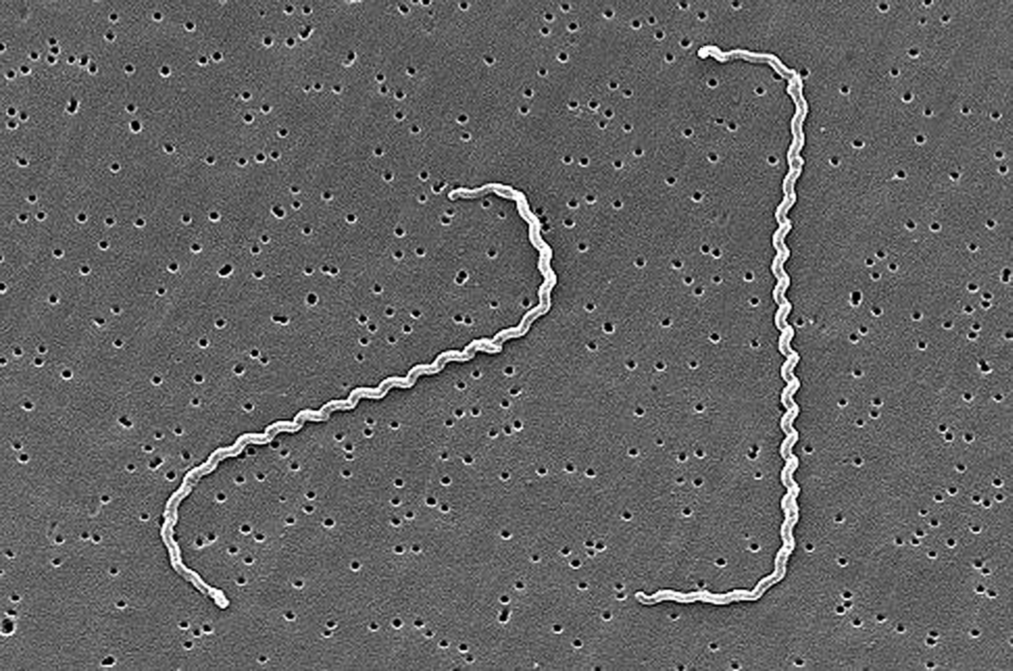
borrelia spp
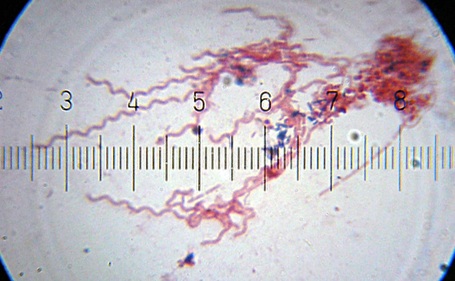
- Thick, GN spirochetes with 3-10 loose coils and 30-40 axial filaments
- Actively motile
- Stain well with Giemsa stain
- Microaerophilic
- Causative agent of tickborne and louseborne relapsing fever and tickborne Lyme disease
- Relapsing fever is caused by B. recurrentis (carried by the louse Pediculus humanus) and B. hermsii, B. turicatae, B. parkeri, and B. bergmanni (carried by the tick of the Orthinodoros spp); Symptoms include an abrupt onset of fever, headache and myalgias after 2-15 days post-infection and lasting 4-10 days; Relapses occur with fever and symptoms, which are milder and shorter in duration
- Lyme Disease is caused by B. burdorferi (carried by the Ixodes pacificus and I. dammini ticks)
- Deer and rodents carry the ticks, as well as domestic pets on occasion
- The tick is the size of a pinhead and must be attached for at least 24 hours before it can transmit disease
- Infections are highest during the Spring and Summer
- Infections are endemic in MA, CT, MD, MN, OR and CA
- Infection occurs by direct invasion of tissues
- IgM antibody complexes are formed against the pathogen, leading to an autoimmune response resulting in the spectrum of disease
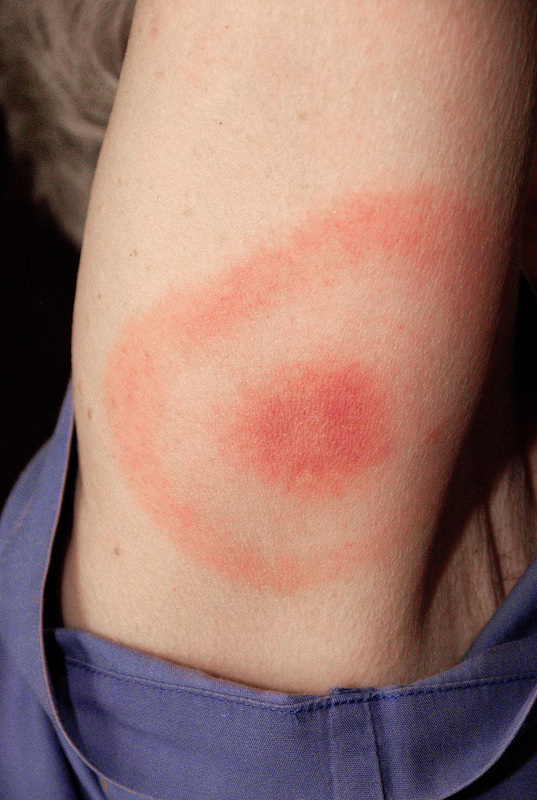
- STAGE I: Erythema migrans (EM)-a characteristic red, ring-shaped/target-shaped skin lesion/rash forms with a central clearing and is accompanied by headache, fever, muscle and joint pain, and malaise
- STAGE II: Weeks-to-months later, arthritis sets in, along with neurological disorders, deficits and meningitis or carditis in some patients
- STAGE III: Chronic arthritis which may last for years or last a lifetime
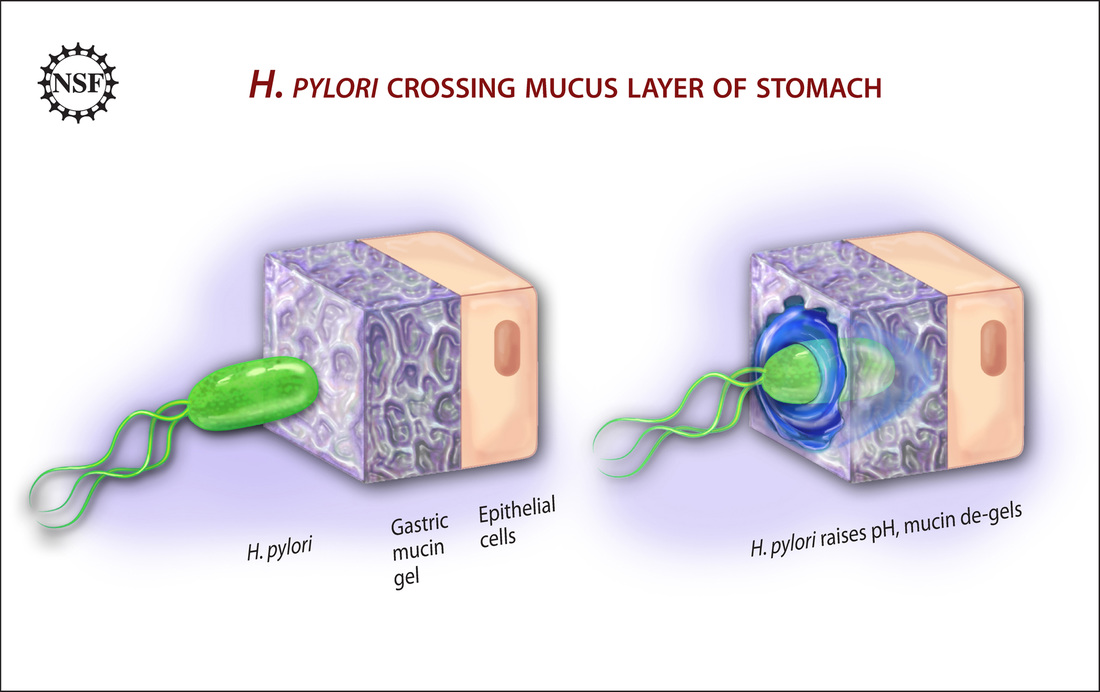
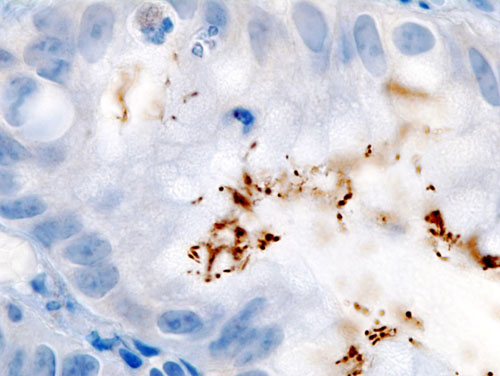
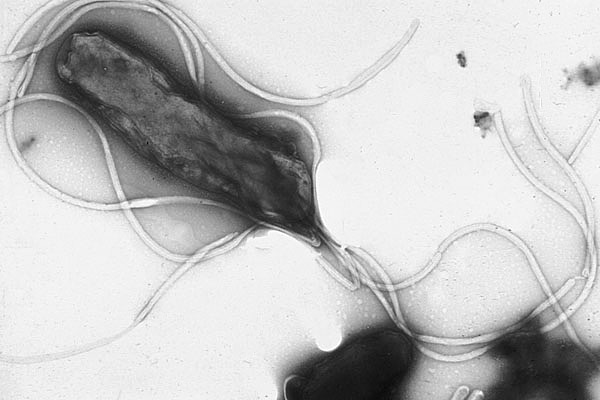
Helicobacter pylori
- H. pylori is a curved/spiral-shaped GN rod
- Microaerophilic
- Strong urease activity
- Primary habitat is the human gastric mucosa
- Motile
- Causes gastritis, peptic ulcer disease, and gastric cancer
- Oxidase and catalase +
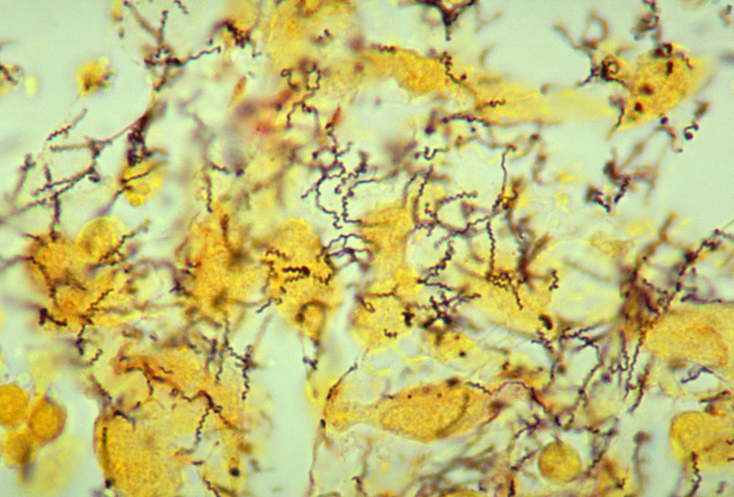
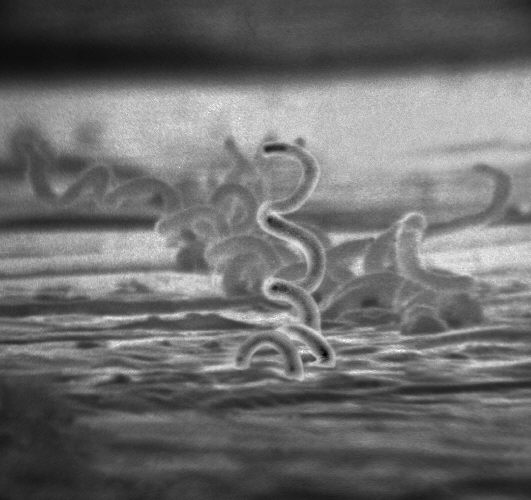
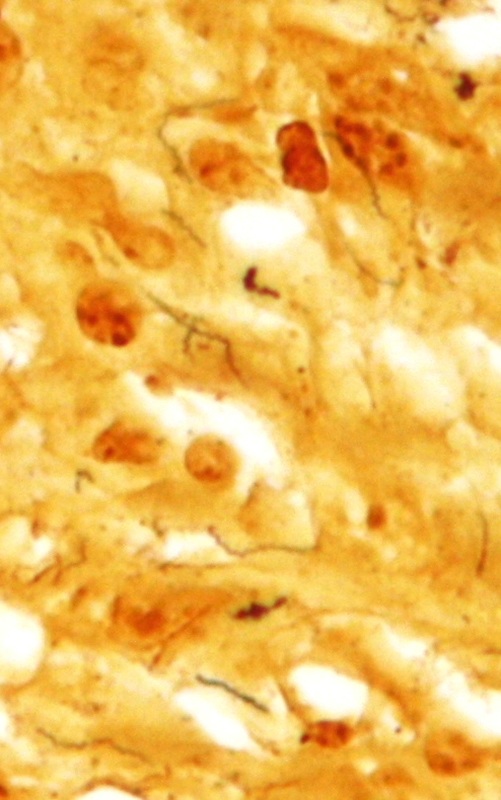
treponema pallidum
- Causative agent of syphilis, an STD
- Slender, GN spirochetes with tight coils and 6-10 axial filaments for motility
- Infects only humans
- May be seen using darkfield, phase-contrast microscopy
- Fails to grow on artificial media or in cell culture
- Microaerophilic
- Penetrates the mucus-membranes or through breaks in the skin
- Enters the bloodstream and spreads to other body sites
- Tropism/attraction to arterioles and infection leads to endarteritis (inflammation of the lining of the arteries)
- Tissue destruction
- Venereal syphilis (Incubating and Primary: chancre, formation of a painless ulcer that heals in 3-6 weeks, followed by dissemination in 2-24 weeks; Secondary: symptoms of illness, including fever, weight loss, malaise, loss of appetite, rash, discharge; Early Latent Stage: Subclinical but not dormant or inactive yet; diagnosis is made by serological testing (VDRL, RPR, FTA-ABS or MHA-TP); Latent Stage: Subclinical, dormant/inactive; Diagnosis made by serological testing; Tertiary Stage: Tissue destruction phase; appears 10-25 years after initial infection in up to 35% of untreated patients; complications may occur involving the CNS, cardiovascular system, eyes, joints, or formation of granuloma-like lesions called gummas in any organ
- Treatment is Penicillin G
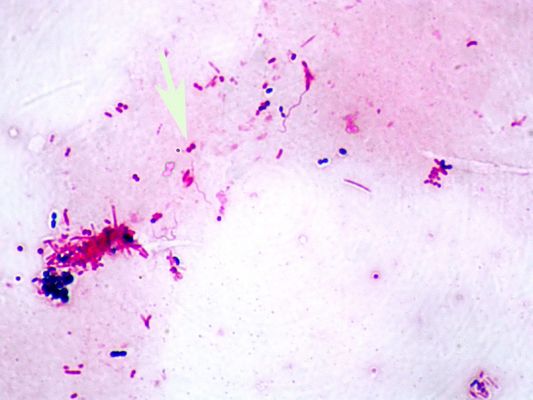
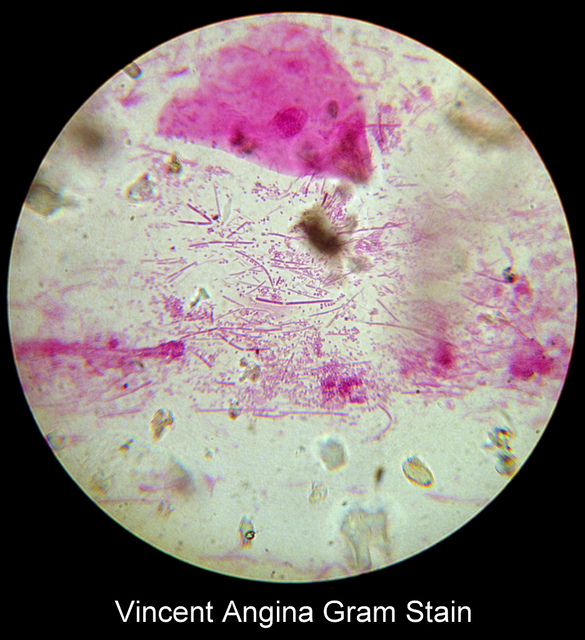
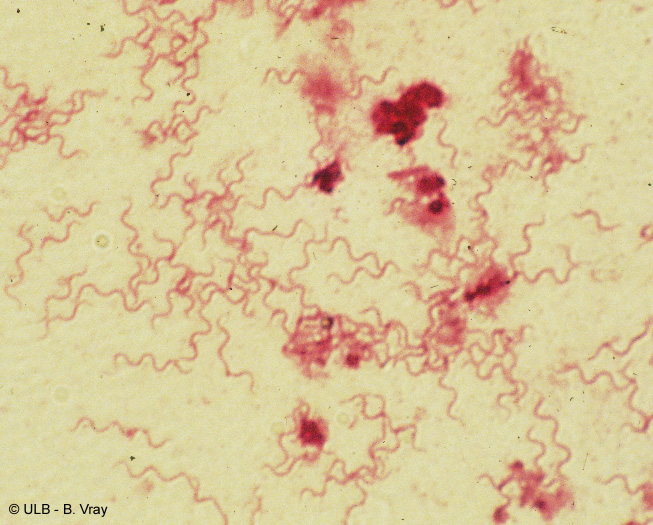
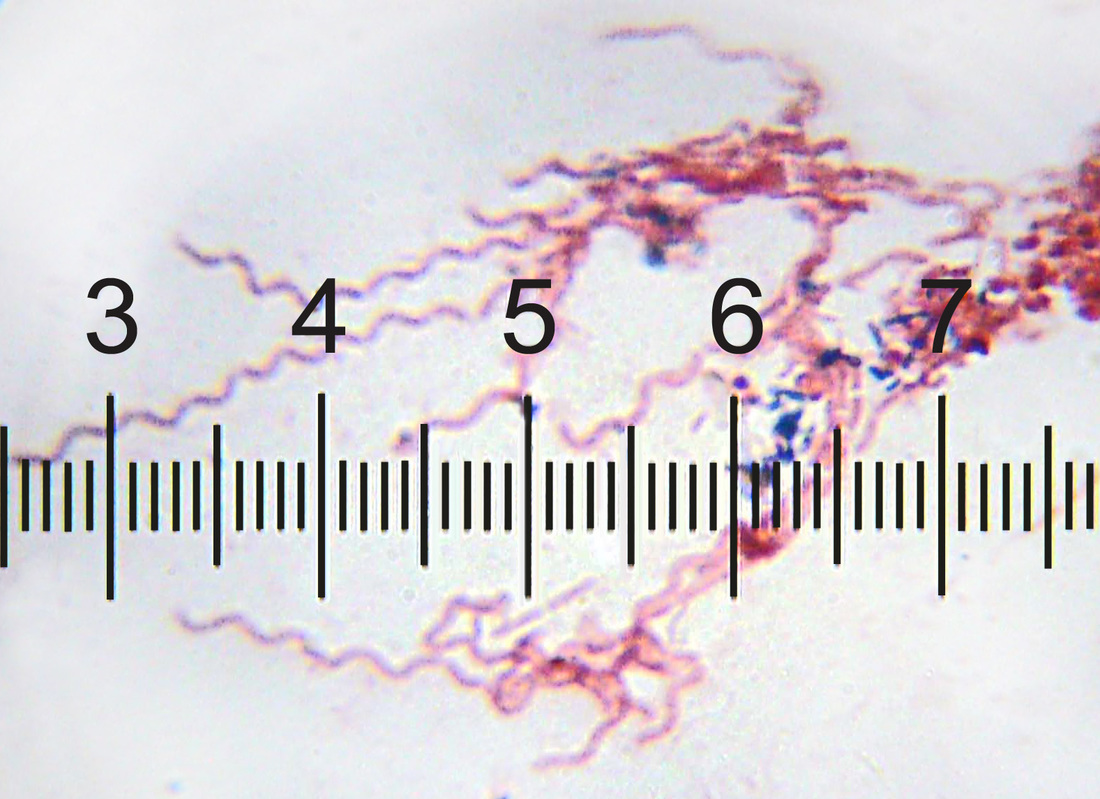
treponema vincentii (borrelia vincentii):
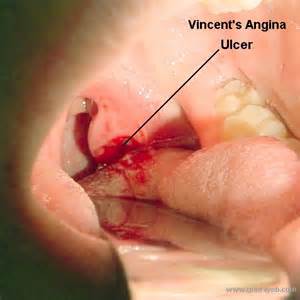
- Causative agent of Vincent's Disease or Vincent's Angina, an ulcerative gingivitis and stomatitis
- When setting up a mouth culture for a dental abscess, this is a wound or anaerobe culture, and in general, most specimens collected from the mouth or oral site are typically poor quality specimens for pathogens and should not be cultured or Gram-stained unless to rule out Vincent's angina or thrush
- The mouth is filled with normal oral flora, both aerobe and anaerobe, including spirochetes, spirilla and fusobacterium
- Scrapings, exudates, and cutterages are OK for culture and the HCP should designate what pathogens are being sought; Ask the reason for the culture
- Gram stain for yeast and/or Vincent's angina are the ONLY appropriate use of mouth swabs; Look for spirochetes, spirilla and fusoform bacteria
- Fusospirochetal Disease
- Occurs with F. nucleatum and F. necrophorum and other anaerobes
- Seen in acute infections and along with white blood cells
- Stain with crystal violet for 1 minute
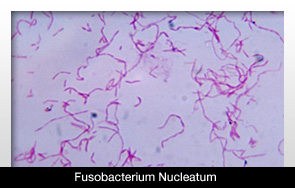
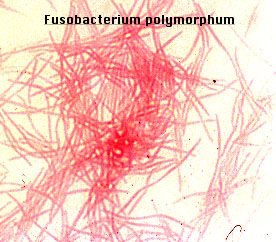
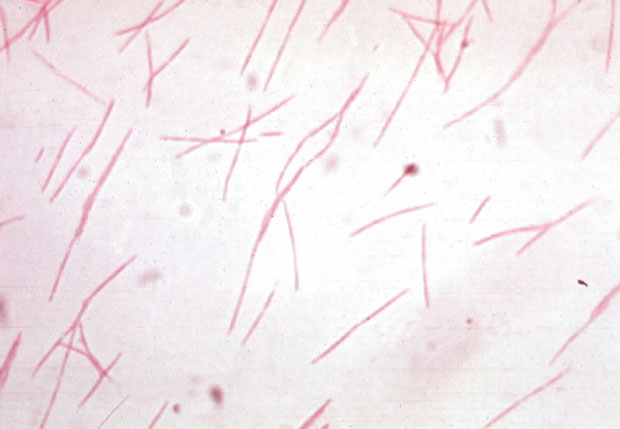
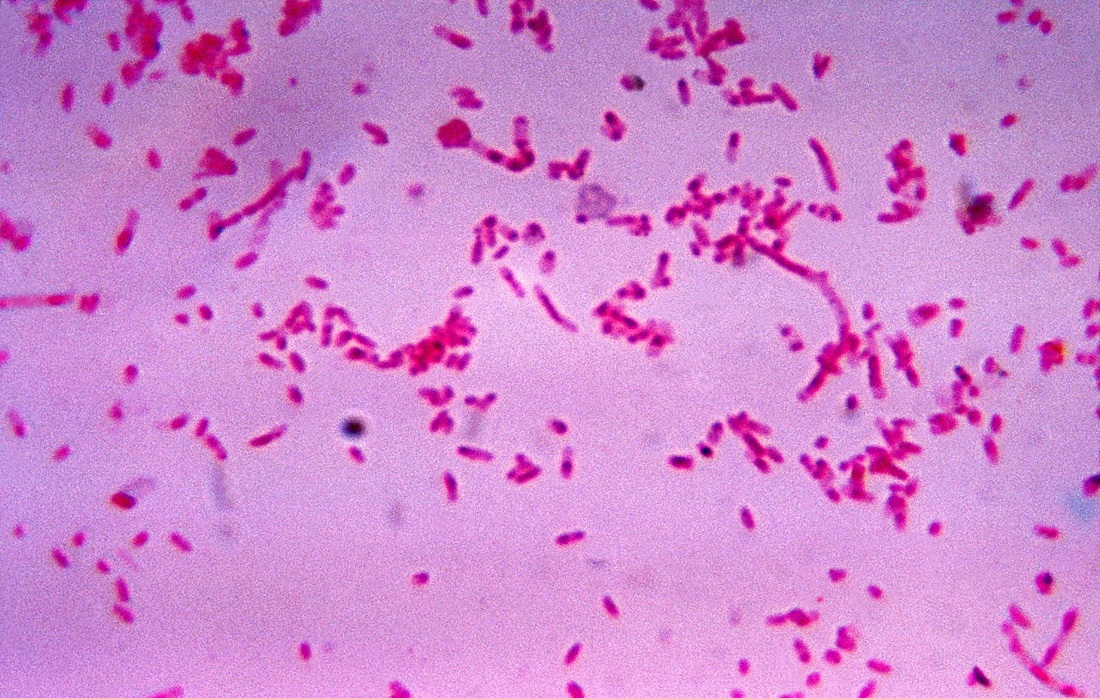
Fusobacterium: fusiform:
- Part of the normal oral flora and gastrointestinal flora
- Opportunistic pathogen and causative agent of polymicrobial abscesses
- Causative agent of Vincent's angina/disease
- Causative agent of Lemierre's Disease
- F. nucleatum
- F. necrophorum
- F. polymorphum
- F. novum
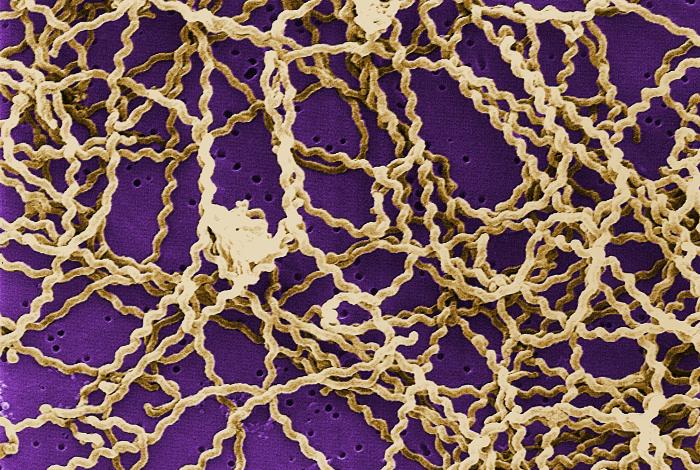
leptospira interrogans
- Causative agent of leptospirosis
- Looks like Borrelia spp, but has hooked ends and 2 axial filaments
- May be recovered on Fletcher's semisolid medium
- Needs an atmosphere of 10% CO2
- Observe with darkfield microscopy (negative stain)
- Free-living forms
- Parasitic forms
- >180 types
- Leptospirosis is a zoonosis found worldwide in infected animals and contaminated water, such as stagnant and polluted water, and wild rodents may carry the spirochete and shed it in their urine and feces (example: rats may carry this organism, and rat-infested areas with water may be a reservoir for infection)
- Enters through the mucus membranes or via breaks in the skin or via the conjunctivae
- Invades the bloodstream and spreads to other body sites (CNS, kidneys, lung)
- Symptoms begin 2-20 days after infection and include fever, headache, myalgias
- May cause liver and kidney failure, with jaundice
- Anicteric Leptospirosis: self-limiting, milder, septic stage with high fever and headache lasting 3-7 days followed by an immune stage and aseptic meningitis
- Icteric Leptospirosis: Weil's syndrome; More severe illness, including the above plus liver, kidney and vascular dysfunction and death in up to 10% of patients
- Blood cultures should be drawn in the first 7-10 days of infection
francisella tularensis
- Causative agent of tularensis or "rabbit fever"
- Very low fatality rate if treated, but can cause severe illness
- Infection may be contracted through direct contact with contaminated fur, inhalation of aerosolized particles, via the fecal-oral route upon ingestion of contaminated water or via insect bites
- It takes just a small number of infectious particles of this organism to cause disease (10-20 microbes)
- Symptoms of illness include fever, severe respiratory illness, life-threatening pneumonia and systemic infection
- The most rapid and specific method of detection of this organism is fluorescent antibody staining techniques
- The best medium for culture of this organism is cystine blood agar
bacillus anthracis
- Causative agent of the disease anthrax, and there are 3 forms: Cutaneous (black eschar formation), Pulmonary (Wool Sorter's Disease), Gastrointestinal (toxemia/sepsis)
- Nonmotile
- Penicillin-susceptible
- Wide zone of lecithinase on egg yolk agar
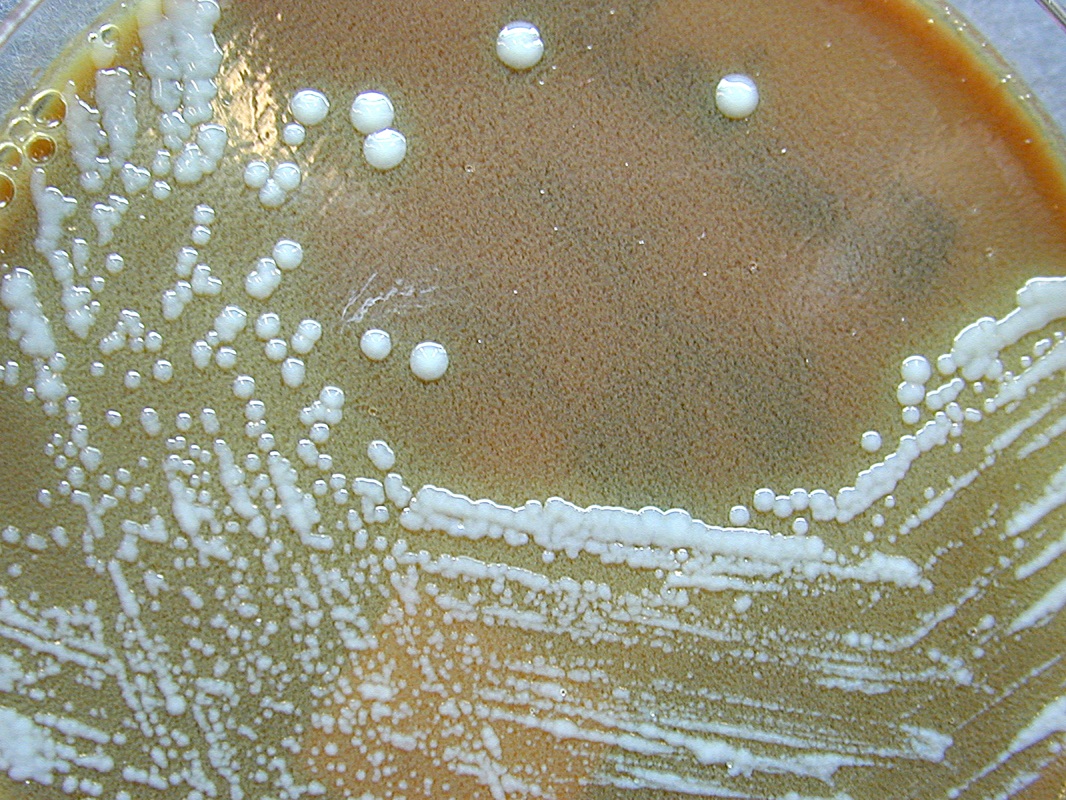
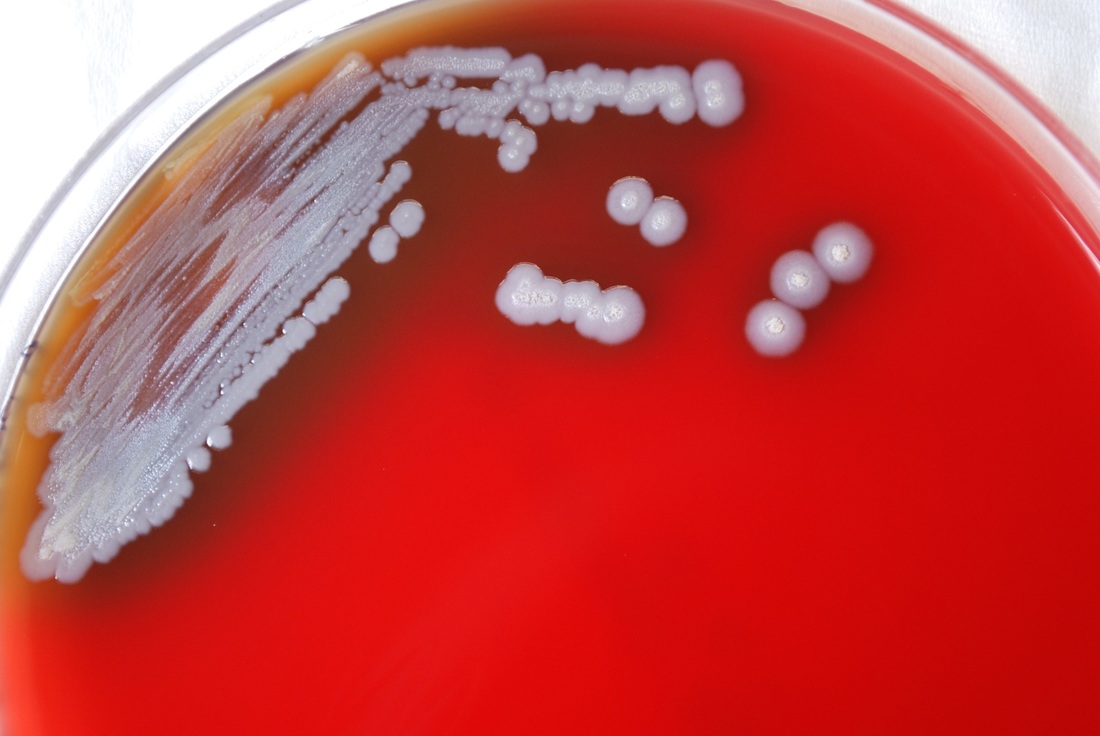
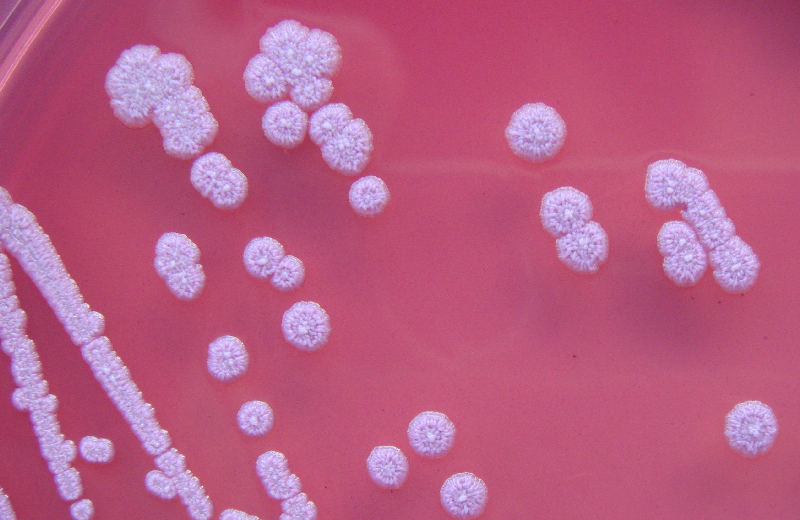
- Growth on sheep blood agar (nonhemolytic, 4-5 mm diameter, off-white with a ground-glass appearance, irregular edges with comma-shaped outgrowths that stand up like "beaten egg whites" when gently lifted with an inoculating needle)
- Negative sugars tests
- Anaerobic growth
- Indole negative
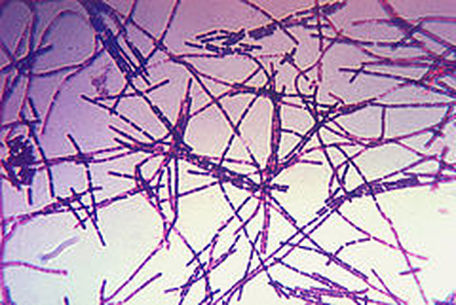
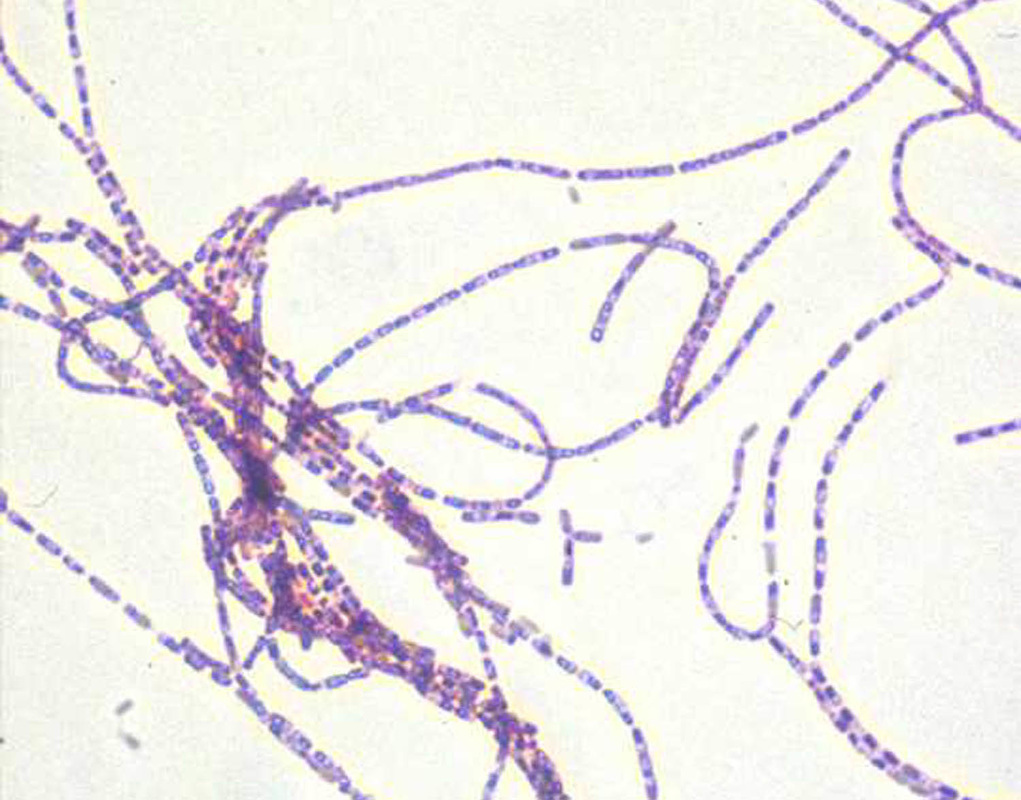
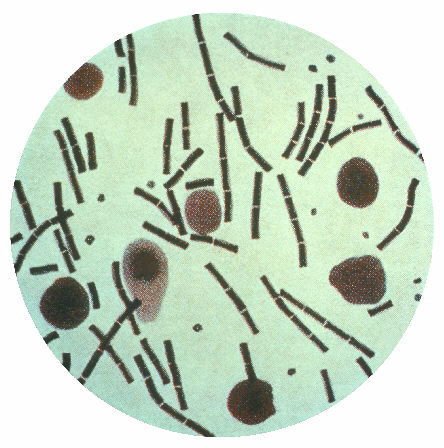
- Disease is caused by the Gram-positive, spore-forming Bacillus anthracis
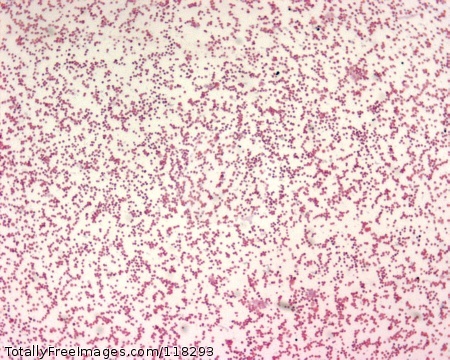
- Bacteria stain Gram-positive when stained from young cultures, but become Gram-variable or Gram-negative with age
- Spores in Gram-stain may appear as clear areas because they do not retain the stain (large, rectangular rods)
- Anthrax vaccine provides protection
- Inhabits the soil
- Humans acquire infection with they are inoculated with the spores during trauma or inhale them during exposure to contaminated animal hides or waste products
- Highly virulent
- Virulence factors include production of an antiphagocytic capsule, potent exotoxins (edema toxin, lethal toxin) that mediate cell and tissue destruction
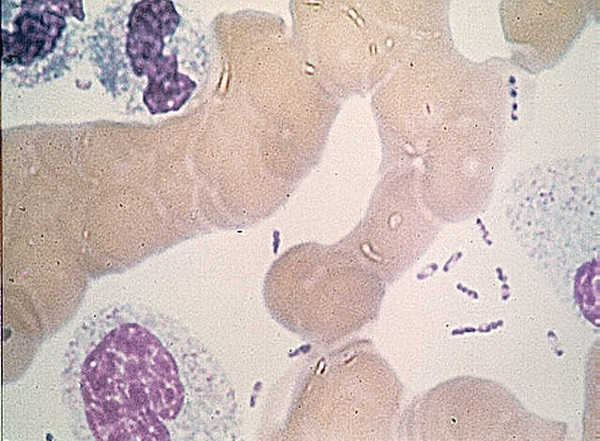
yersinia pestis
- Causative agent of bubonic plague and pneumonic plague
- Rodents are the hosts/reservoirs, and can transmit the disease to humans via flea bites (bubonic plague) or aerosolized particles (pneumonic plague)
- Prairie dogs are known to carry this organism
- Caused the "Black Death" during the medieval times in Europe
- Illness causes a high fever, diarrhea, and prostration with enlarged and hemorrhagic axillary lymph nodes
- This organism is a Gram-negative bacilli that stains bipolar like a "safety-pin" with Wayson's stain
brucella
- Causative agent of brucellosis
- Humans acquire infection from direct contact with infected animal meat or ingestion of contaminated milk products
- Penetrates the skin, conjunctiva, lungs or GI tract
- Spreads through the lymphatic system
- Facultative intracellular growth in macrophages
- Symptoms: systemic (fever, chills, sweating, loss of appetite, aches and pains, headache, lymphadenopathy)
- Undulant fever
- If recovered in blood culture bottle the bottle should be held for 21 days
burkholderia mallei
- Causative agent of glanders
burkholderia pseudomallei
- Causative agent of melioidosis
legionella pneumophila
Legionella pneumophila is the causative agent of Legionnaire's Disease (epidemic pneumonia). This bacteria is a faintly staining, thin Gram-negative bacillus that requires both L-cysteine and a pH of 6.9 to grow. Most are motile. There are 40+ spp of Legionella. The bacterium prefers a moist, warm, aquatic environment to grow in (lakes, rivers, streams, marine waters, moist soil, air-conditioning ducts, cooling towers, humidifiers, large, warm water plumbing systems, whirlpools, hospital medical equipment such as nebulizers, showers, and warm tap water). It is a facultative intracellular pathogen that thrives in alveolar macrophages. There are three clinical manifestations:
1) Pneumonia, with a fatality of 10-20%: Legionnaire's Disease
2) Pontiac Fever, a self-limited, non-fatal respiratory infection
3) Wound abscesses, encephalitis, or endocarditis.
The disease is diagnosed through Giemsa stains, DFA, urine assays, positive blood cultures or PCR. It grows well on BCYE agar, which is based with charcoal to detoxify. This bacterium is biochemically inert. The organism is a slow-grower and may be cultured on Buffered Charcoal Yeast Extract agar (BCYE) and observed for 7 days. The microbe is characteristically oxidase +, catalase +, replicates inside macrophages, requires cysteine and iron to grow, and forms gray, "cut glass" colonies that look opal-like on the BCY# agar.
1) Pneumonia, with a fatality of 10-20%: Legionnaire's Disease
2) Pontiac Fever, a self-limited, non-fatal respiratory infection
3) Wound abscesses, encephalitis, or endocarditis.
The disease is diagnosed through Giemsa stains, DFA, urine assays, positive blood cultures or PCR. It grows well on BCYE agar, which is based with charcoal to detoxify. This bacterium is biochemically inert. The organism is a slow-grower and may be cultured on Buffered Charcoal Yeast Extract agar (BCYE) and observed for 7 days. The microbe is characteristically oxidase +, catalase +, replicates inside macrophages, requires cysteine and iron to grow, and forms gray, "cut glass" colonies that look opal-like on the BCY# agar.