Oral hygiene, Antimicrobial Bathing, and Cleaning Blood culture bottles and patient skin: Preventing normal microflora from getting into the wrong place at the wrong time
Oral hygiene is important, not just so that we have fresh breath and clean teeth, but also to prevent bacterial endocarditis, heart disease due to plaque formation and inflammation in the heart, and ventilator-associated pneumonia in patients who are on ventilators in the hospital, particularly in the ICU.
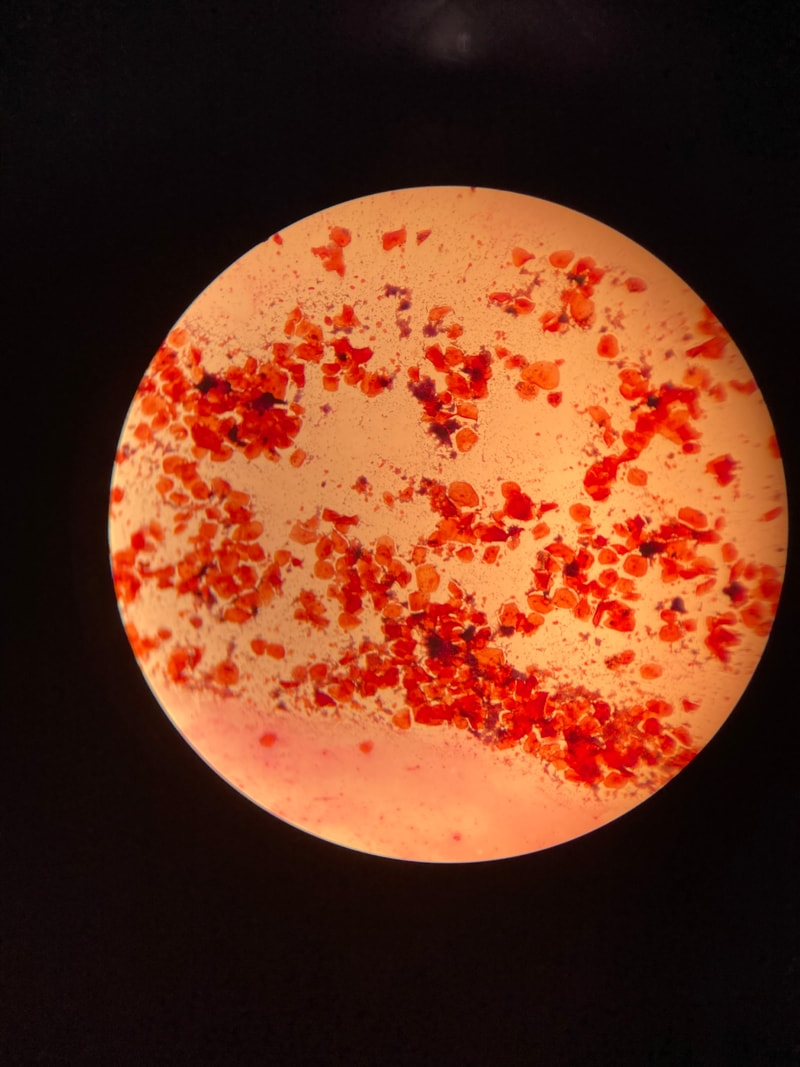
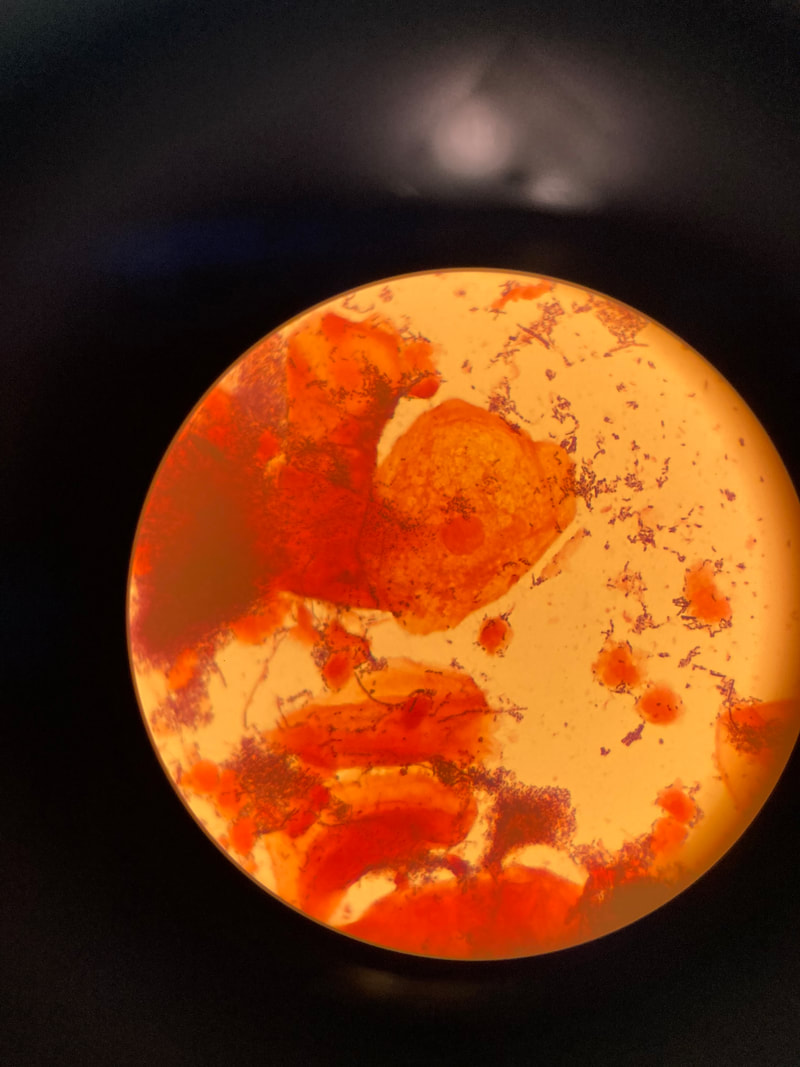
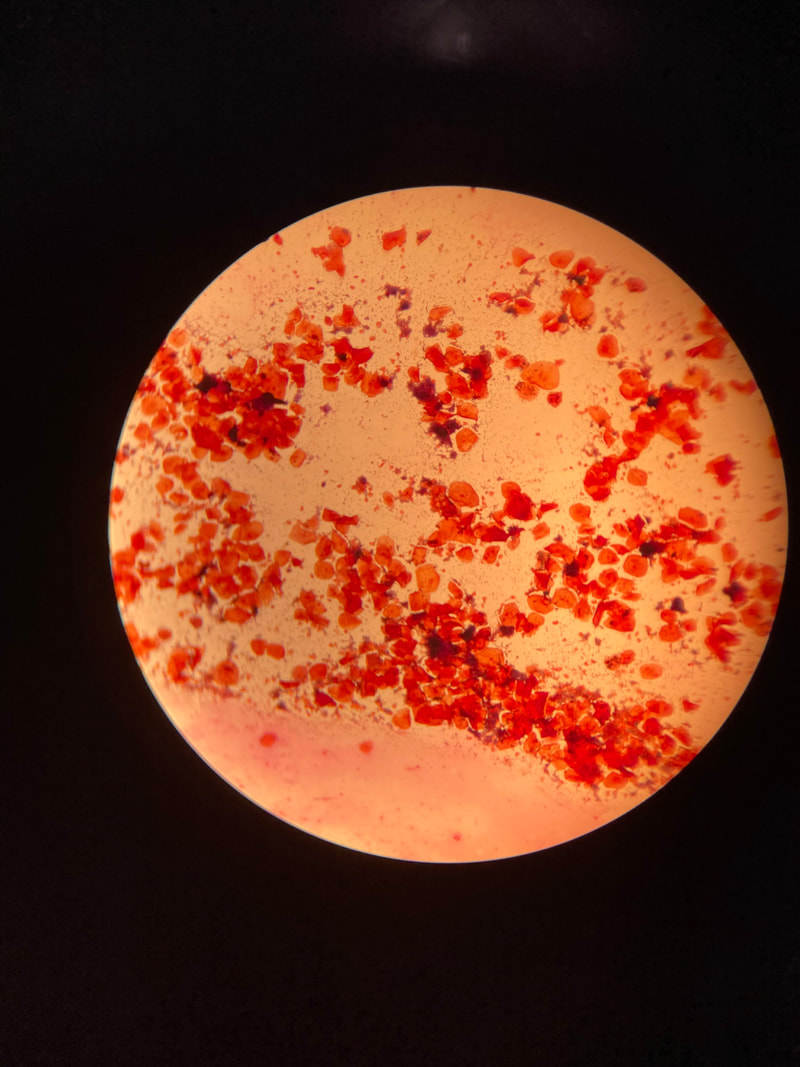
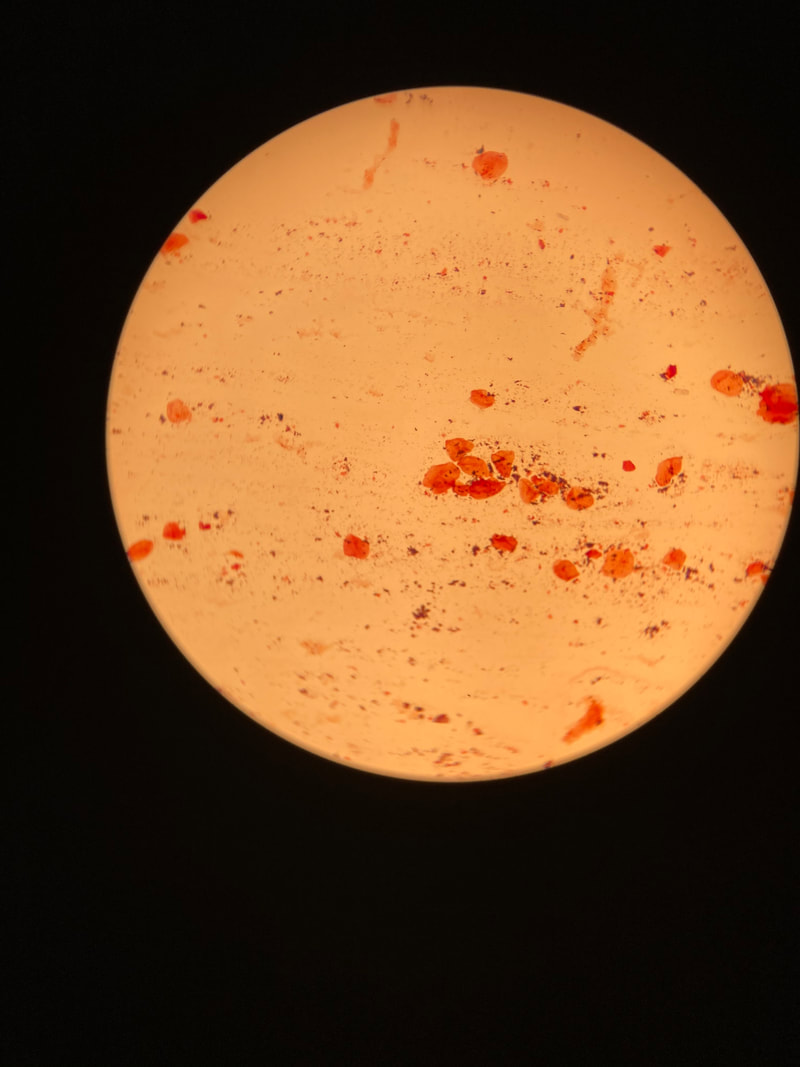
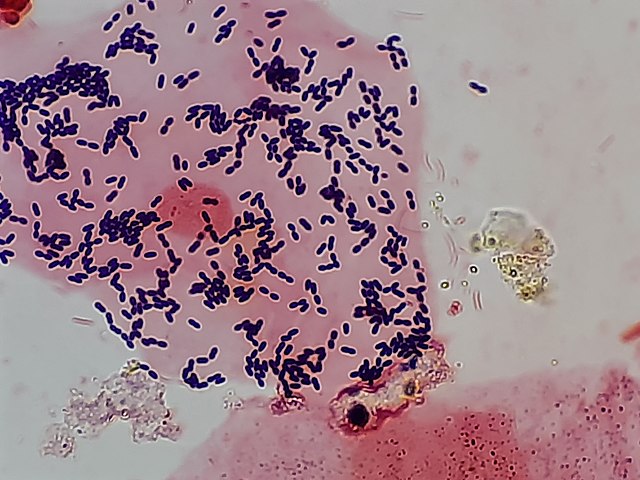
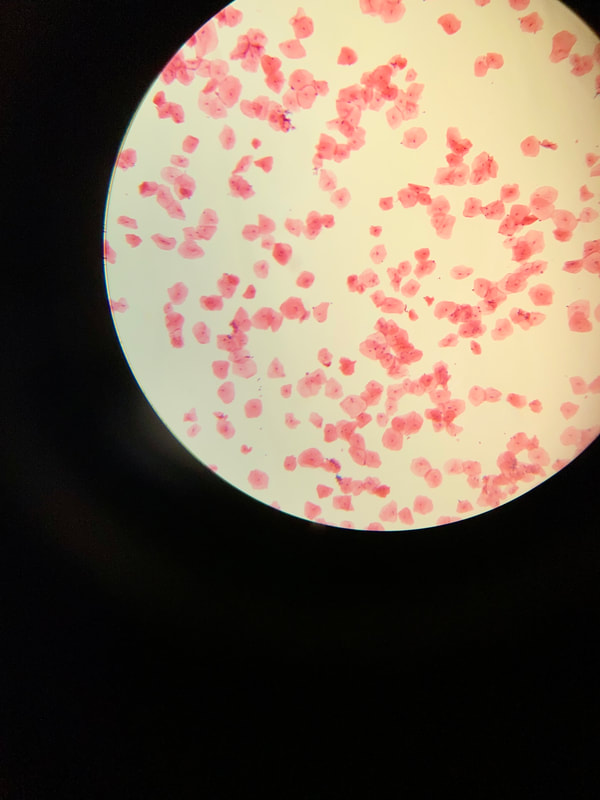
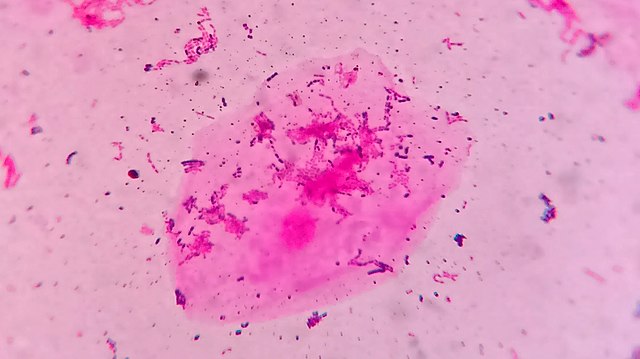
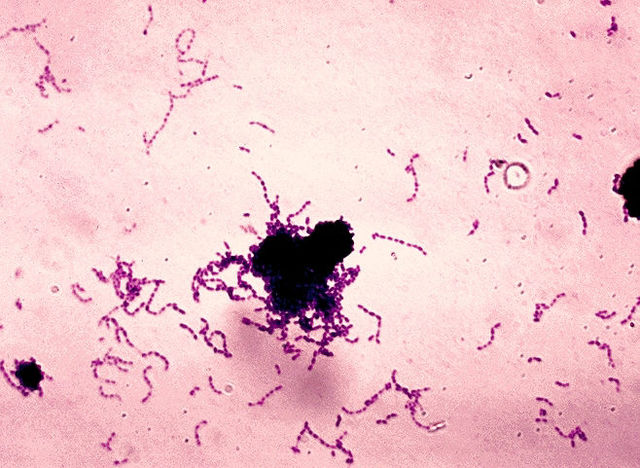
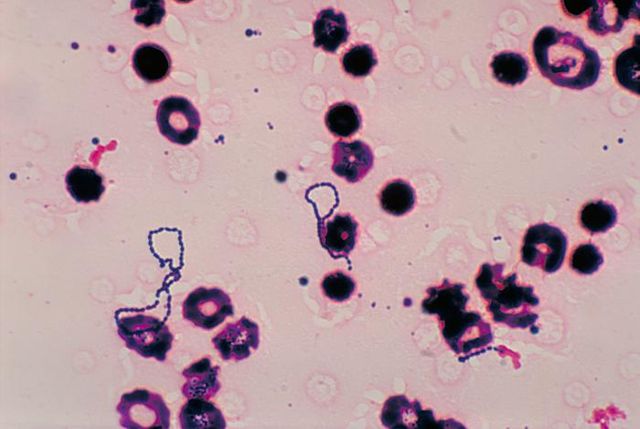
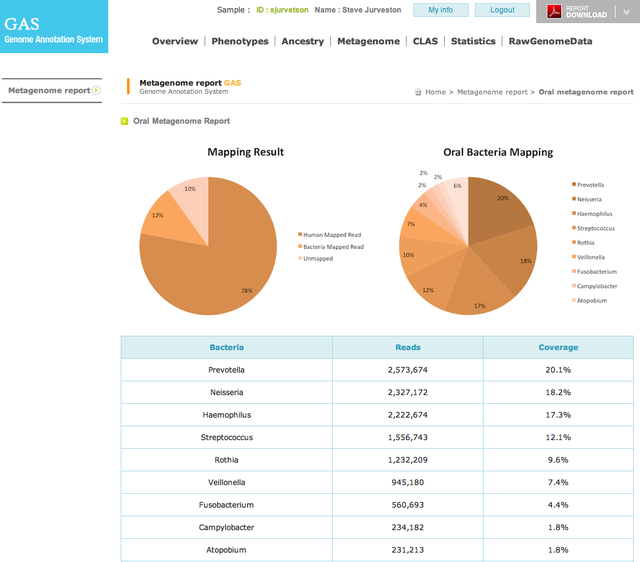
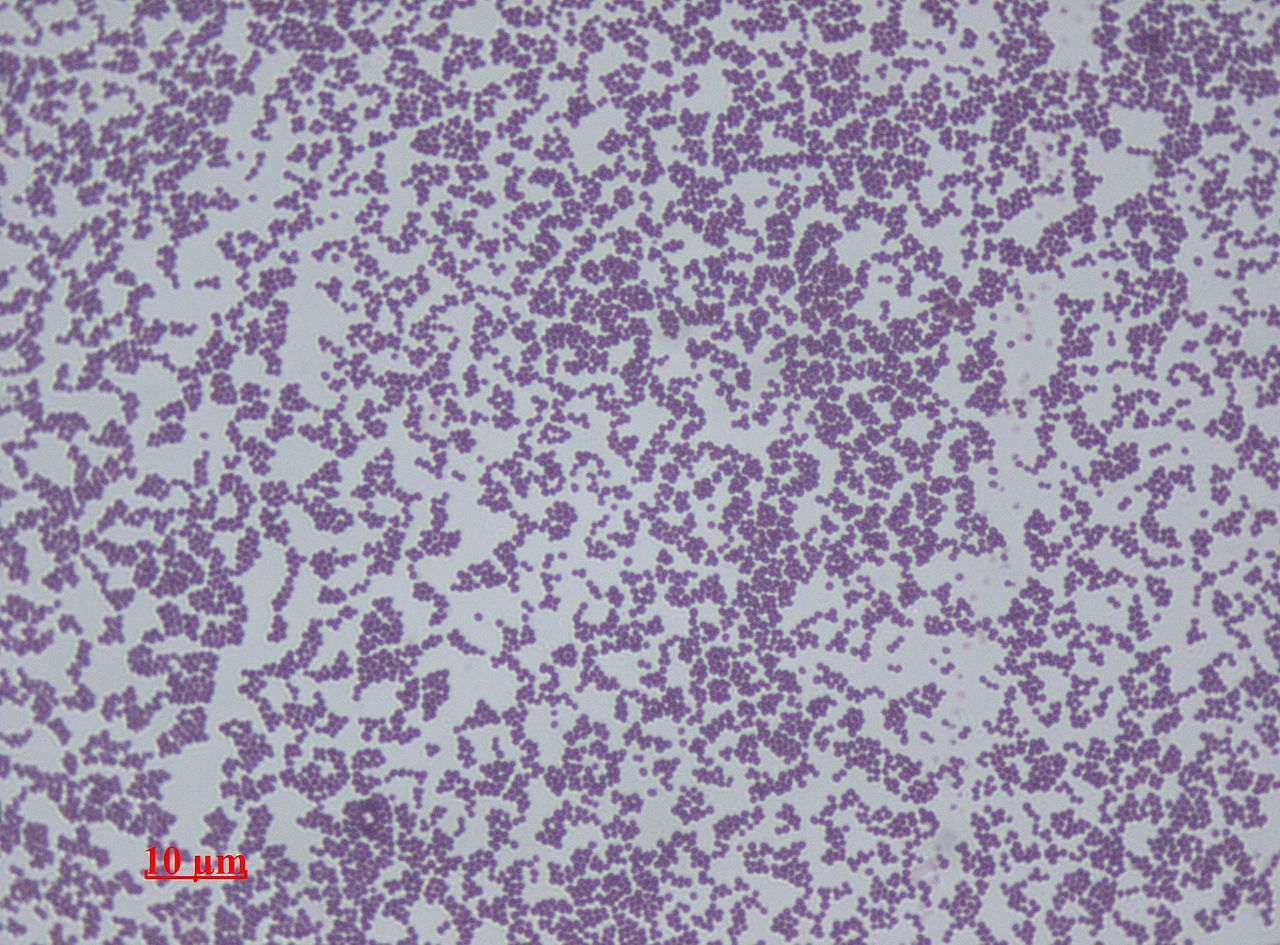
Below are some images of the bacteria found in our mouths and mucous membranes and skin. This is called the normal microflora. We are colonized internally and externally with about 200 trillion different types of bacteria and other microbes, however, if they get into the wrong place at the wrong time, this can lead to opportunistic infections, including aspiration pneumonia, skin and soft tissue or wound infections, or worse. In the hospital, this is why patient oral care, patient bathing and CHG bathing with chlorhexidine or Hibiclens, and thoroughly cleaning a patient's skin prior to performing venipuncture or a surgical procedure are keys to preventing infection by reducing the levels of microbes on the skin to safer levels.
This is also why it is so important to thoroughly cleanse the patient's skin prior to collecting blood or giving an injection. IF the skin is not cleansed properly first, and if the blood culture bottle tops are not cleansed properly first, it can lead to false positive alarms due to contamination of the blood culture with normal skin flora. It is also important to properly teach people to follow the steps of wiping 3x with antiseptic wipes prior to collecting urine for urine cultures, because urine cultures will grow contaminated cultures if the skin is not properly cleansed prior to collecting urine for culture and urinalysis.
Below are some images of the bacteria found in our mouths and mucous membranes and skin. This is called the normal microflora. We are colonized internally and externally with about 200 trillion different types of bacteria and other microbes, however, if they get into the wrong place at the wrong time, this can lead to opportunistic infections, including aspiration pneumonia, skin and soft tissue or wound infections, or worse. In the hospital, this is why patient oral care, patient bathing and CHG bathing with chlorhexidine or Hibiclens, and thoroughly cleaning a patient's skin prior to performing venipuncture or a surgical procedure are keys to preventing infection by reducing the levels of microbes on the skin to safer levels.
This is also why it is so important to thoroughly cleanse the patient's skin prior to collecting blood or giving an injection. IF the skin is not cleansed properly first, and if the blood culture bottle tops are not cleansed properly first, it can lead to false positive alarms due to contamination of the blood culture with normal skin flora. It is also important to properly teach people to follow the steps of wiping 3x with antiseptic wipes prior to collecting urine for urine cultures, because urine cultures will grow contaminated cultures if the skin is not properly cleansed prior to collecting urine for culture and urinalysis.
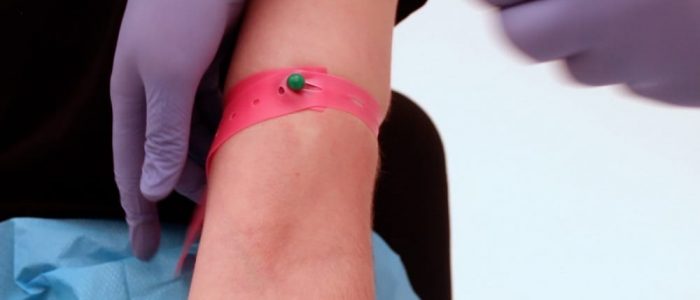
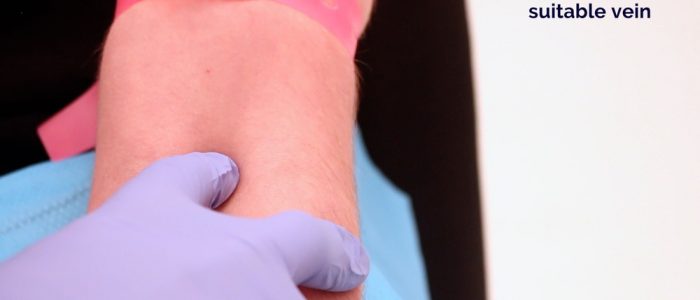
cleaning the patient's skin prior to venipuncture:
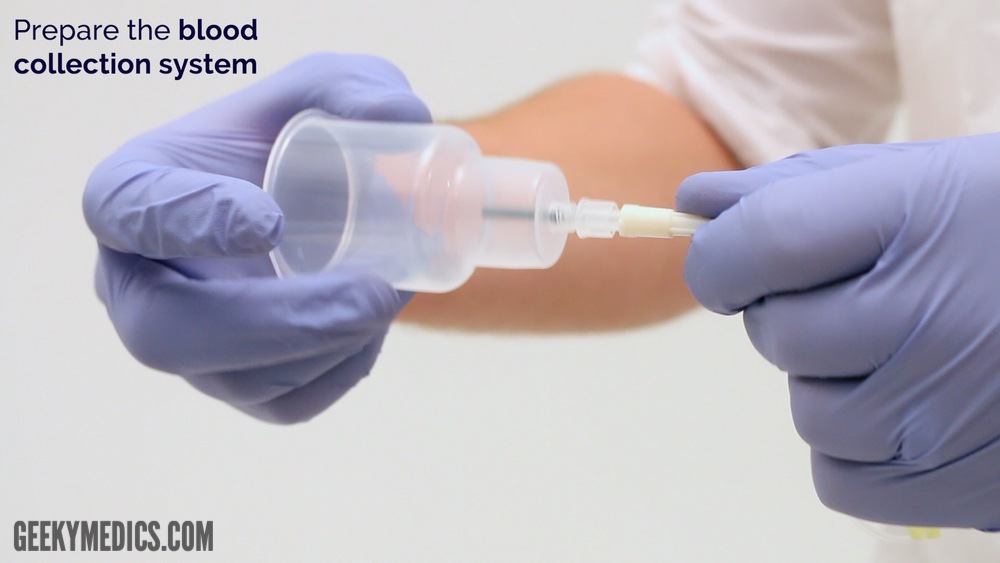
When preparing to collect blood, once an ideal site has been chosen, release the tourniquet. It is important not to keep the tourniquet tightened for more than 60 seconds, or all the metabolites will become too concentrated, leading to false elevations and test results. 70% isopropyl alcohol solution applied with sterile gauze, a cotton ball or swab or the use of alcohol wipes are used to clean and disinfect the patient's skin prior to performing venipuncture or to inserting an IV line or otherwise puncturing the skin for a medical procedure. It is important to put enough pressure on the skin to disinfect it, firm yet gentle, along with going in concentric circles (small inner circles from the center of where the venipuncture is to be performed, to larger outer circles). You want to move out at least 2 cm, allowing it to completely air dry. DO NOT blow on it, or you will break the disinfection you just completed by contaminating with the breath. Don't go back over any area of the skin once it has been cleansed. If the skin is not completely dry, the alcohol will cause the blood cells to hemolyze, interfering with the testing and results. Allow for 15-20 seconds for the skin to dry. Avoid touching this site.
When collecting blood for blood cultures, extra measures need to be taken for cleansing the skin AND the collection bottles prior to the actual collection. This includes cleaning the skin THREE TIMES with a povidone-iodine solution or a chlorhexidine gluconate preparation. By using a scrub applicator, the solution must be applied to the puncture site in a concentric, outward circle, starting at the site. It is critical that this step is repeated THREE TIMES. After the triple cleaning step, the povidone-iodine may be removed with a 70% isopropyl alcohol pad or 70% isopropyl alcohol solution on a sterile cotton ball, swab or piece of gauze. If the phlebotomist or RN drawing the blood needs to palpate the vein again, their gloved hand should ALSO be triple-cleaned with the povidone iodine solution before palpating the vein. The venipuncture should be performed using a sterile syringe and needle, or collected directly into the blood culture bottles using an evacuated (vacuum) system.
When collecting blood for blood cultures, extra measures need to be taken for cleansing the skin AND the collection bottles prior to the actual collection. This includes cleaning the skin THREE TIMES with a povidone-iodine solution or a chlorhexidine gluconate preparation. By using a scrub applicator, the solution must be applied to the puncture site in a concentric, outward circle, starting at the site. It is critical that this step is repeated THREE TIMES. After the triple cleaning step, the povidone-iodine may be removed with a 70% isopropyl alcohol pad or 70% isopropyl alcohol solution on a sterile cotton ball, swab or piece of gauze. If the phlebotomist or RN drawing the blood needs to palpate the vein again, their gloved hand should ALSO be triple-cleaned with the povidone iodine solution before palpating the vein. The venipuncture should be performed using a sterile syringe and needle, or collected directly into the blood culture bottles using an evacuated (vacuum) system.
Cleaning a blood culture bottle:
The accuracy of laboratory tests starts with the quality of the specimen collection and receipt by the laboratory. How the sample is collected, transported and processed matters tremendously and each person's role in this process is critical. If the sample is improperly collected, stored or mishandled, this means the sample will be invalid and cannot be used by the physician for diagnosis or treatment. Recollections, delayed turnaround time, results in delayed diagnosis and treatment, and may also result in extended hospital stays in some cases. Quality sample collection includes multiple measures that must be followed and monitored for a patient's safety:
Phlebotomists and nurses that collect blood are crucial steps to patient care, testing, diagnosis and treatment. Most laboratory errors actually start with mistakes before testing, which are preanalytical errors, many of which are related to specimen collection and handling. Being well-trained can aid in reducing these mistakes and increase a constant alertness to sources of error. Professionalism and delivery of excellent customer service and satisfaction is also key.
Blood is often one of the first samples collected in the hospital or clinical setting, and often one of the first analyzed in the clinical laboratory. Knowledge of proper collection, preservation, and processing of blood and other samples is essential. A properly collected blood sample is critical to quality performance in the laboratory. Strict adherence to the rules of specimen collection should be followed for accuracy.
Blood samples may be collected by health care personnel with different skills and educational backgrounds. An increased emphasis on safety is key when collecting blood and other samples. BD Vacutainers, safety lancets, needleless systems, safety devices, and transfer devices aid in safety for everyone when collecting blood. When collecting blood, it is important to follow the order of the draw. This section focuses specifically on the collection of blood cultures, which are collected first if they are ordered. Blood culture bottles may be aerobic, anaerobic, and/or pediatric. They additive inside the bottles is STERILE, meaning that they contain no microbes. When you pop the top off a brand new blood culture bottle, however, it is so important to realize that this part IS NOT completely sterile. There could be dust and microbes on the rubber piece that was under the cap. It is so important to disinfect the blood culture bottle top with a 70% isopropyl alcohol pad prior to injecting the required amount of blood sample into the blood culture bottle(s) to prevent blood culture bottle contamination, leading to false positive results, and potential unnecessary treatment of a patient.
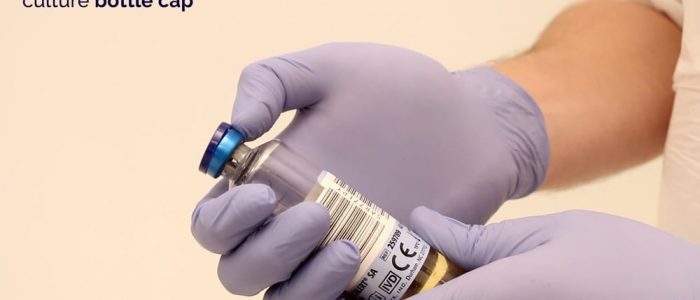
The top of the blood culture bottle should be cleansed using a 2% chlorhexidine in 70% isopropyl alcohol wipe before you begin the process of blood collection. This process should be followed EVERY single time for EVERY single bottle. You should be wearing gloves when performing this process. If you are using a transfer device, make sure you are using aseptic technique and caution to prevent an accidental needlestick.
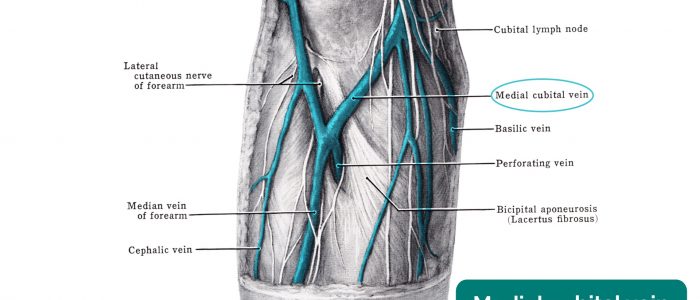
There are some special site selection situations in the hospital setting, in particular, to be aware of when collecting blood cultures.
- Preparing the patient for sample collection, including acknowledging them, introducing yourself, describing what you are going to be doing and the duration of the procedure, explaining the procedure or process, and thanking them for allowing you to collect the sample
- Collection of a valid quality sample
- Proper transport of the specimen
- Following through with the requested order and laboratory test
- Validation of the test results
- Recording and reporting of the test results
- Transmitting the test results to the patient's medical record
- Documenting, maintaining, and properly charting records in a timely manner, including quality assessment practices and quality control measures
Phlebotomists and nurses that collect blood are crucial steps to patient care, testing, diagnosis and treatment. Most laboratory errors actually start with mistakes before testing, which are preanalytical errors, many of which are related to specimen collection and handling. Being well-trained can aid in reducing these mistakes and increase a constant alertness to sources of error. Professionalism and delivery of excellent customer service and satisfaction is also key.
Blood is often one of the first samples collected in the hospital or clinical setting, and often one of the first analyzed in the clinical laboratory. Knowledge of proper collection, preservation, and processing of blood and other samples is essential. A properly collected blood sample is critical to quality performance in the laboratory. Strict adherence to the rules of specimen collection should be followed for accuracy.
Blood samples may be collected by health care personnel with different skills and educational backgrounds. An increased emphasis on safety is key when collecting blood and other samples. BD Vacutainers, safety lancets, needleless systems, safety devices, and transfer devices aid in safety for everyone when collecting blood. When collecting blood, it is important to follow the order of the draw. This section focuses specifically on the collection of blood cultures, which are collected first if they are ordered. Blood culture bottles may be aerobic, anaerobic, and/or pediatric. They additive inside the bottles is STERILE, meaning that they contain no microbes. When you pop the top off a brand new blood culture bottle, however, it is so important to realize that this part IS NOT completely sterile. There could be dust and microbes on the rubber piece that was under the cap. It is so important to disinfect the blood culture bottle top with a 70% isopropyl alcohol pad prior to injecting the required amount of blood sample into the blood culture bottle(s) to prevent blood culture bottle contamination, leading to false positive results, and potential unnecessary treatment of a patient.
The top of the blood culture bottle should be cleansed using a 2% chlorhexidine in 70% isopropyl alcohol wipe before you begin the process of blood collection. This process should be followed EVERY single time for EVERY single bottle. You should be wearing gloves when performing this process. If you are using a transfer device, make sure you are using aseptic technique and caution to prevent an accidental needlestick.
There are some special site selection situations in the hospital setting, in particular, to be aware of when collecting blood cultures.
- A limb with an IV line running in it should not be used for venipuncture due to contamination to the specimen. The other arm or an alternate site should be selected.
- If there is an area with extensive scarring or burns, alternate sites or capillary blood collection should be used.
- Blood should not ever be drawn from a vein in an arm with a cannula (for dialysis) or fistula (permanent surgical fusion of a vein and artery) unless the staff is specially trained to draw blood from a cannula. The preferred site is a hand vein or vein away from the fistula or the underside of the arm.
- If a mastectomy patient has had lymph nodes removed, venipuncture should not be performed on that same side.
- Blood cultures need to be drawn BEFORE the patient starts on antibiotics.
Steps to cleaning a blood culture bottle:
- Wash your hands thoroughly using good hand hygiene with soap and water for 20 seconds, and pat them dry with a fresh, clean paper towel.
- Don a fresh, clean pair of gloves.
- Use AIDET and gain patient consent for the procedure. Find out if they have any allergies, such as latex allergies.
- Remove the plastic caps from the bottle tops while wearing fresh, clean gloves that you've just donned.
- Clean the rubber septum on the top with 70% isopropyl alcohol, and allow to completely air dry.
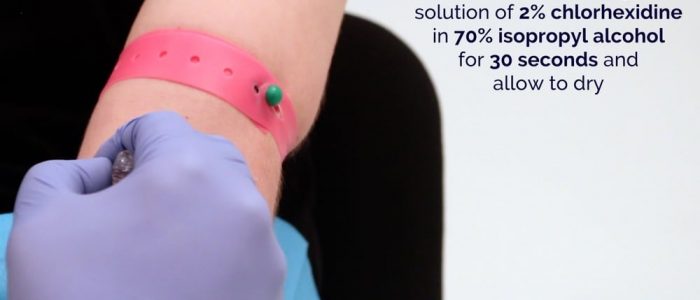
- Firmly, yet gently, prepare the patient's skin and venipuncture site by cleansing for 30 seconds with povidone-iodine or chlorhexidine preps in concentric circles. Repeat this process 3x. Follow with a 70% isopropyl alcohol wipe. Allow to air dry.
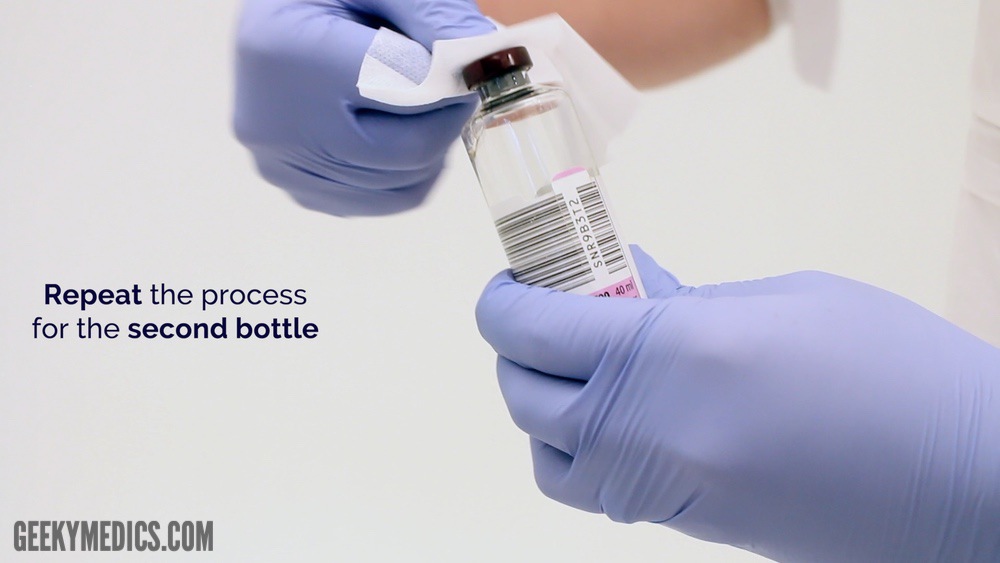
- Clean each bottle with separate chlorhexidine preparations (2% in 70% isopropyl alcohol), allowing them to completely air dry.
- Scrub the tops with a separate 70% isopropyl alcohol wipe each for 30 seconds and allow to air dry. Do not blow on, touch or "fan" the area to help dry it.
preparing the patient for venipuncture:
preparing the blood culture bottles for collection:
when you label the culture bottles, never cover this bar code. This is the part the incubator needs to read.
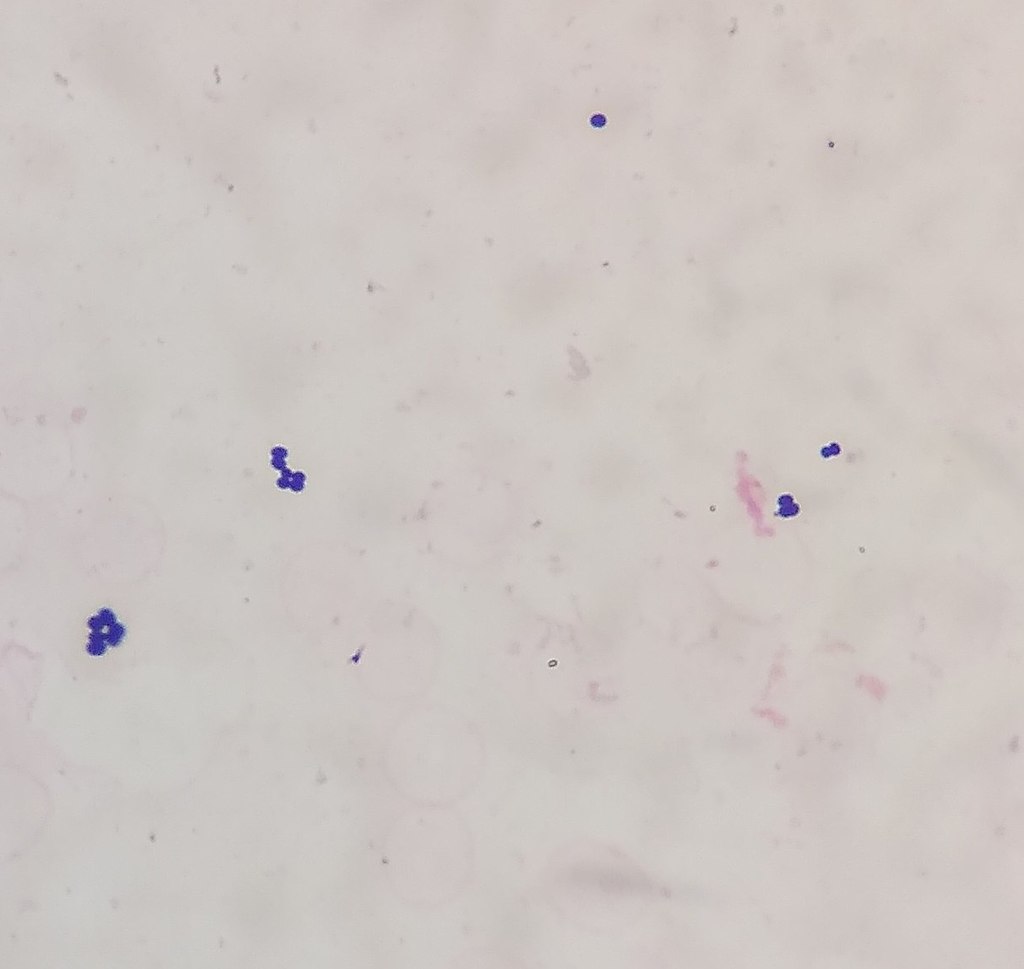
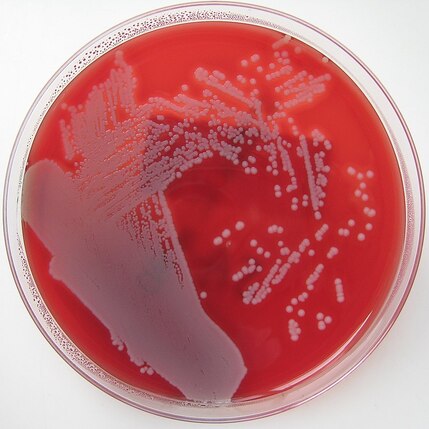
example positive bottle growing staphylococcus aureus on initial gram-stain and subculture to trypticase soy agar with 5% sheep's blood:
NOTE: This is a helpful hint for when you have a positive blood culture bottle, but you don't see anything on the Gram stain. You can cytocentrifuge the blood to concentrate it, then perform another Gram stain. Always look around the edges of the slide, because many times, the bacteria will be found along the edges and you can often see in concentrate what you couldn't see in the initial slide.
Another helpful hint is that blood cultures will come up positive when there is leukocytosis, or a high white blood cell count, even if no bacteria is present.
Another helpful hint is that blood cultures will come up positive when there is leukocytosis, or a high white blood cell count, even if no bacteria is present.
this is an example of a bac-t alert blood culture incubator. bactec is another common type.
The reason a set of blood cultures is drawn at different times is to make sure that any microbes that are present in the bloodstream, if present, will be captured. Aerobic bottles help organisms that need oxygen to grow. Anaerobic bottles help organisms grow that are poisoned by the presence of oxygen. There is a broth inside the bottles, an anticoagulant to prevent clotting, known as sodium polyanethol sulfonate (SPS), and anerobic bottles often include thioglycollate as well. If an organism only grows in one bottle or one of the two sets, it is less likely to be true bacteremia and more likely to simply be a contaminant with microflora from the skin.
A false positive can occur if the blood culture bottle is contaminated with skin flora. A false negative can occur if the patient started antimicrobials before the blood culture bottles were drawn, or if not enough blood was drawn so the blood-to-broth ratio is too low. Blood culture bottles are placed in an incubator, as seen above, which maintains them at a specific temperature and gently shakes them for up to 7 days (longer for fungal and AFB bottles). There are carbon dioxide sensors on the bottom that sense gases produced by microbes during the fermentation process. There is sterile broth with nutrients inside the bottles.
If the machine alarms, the blood culture bottle is removed and a Gram-stain is performed (initial) to look for microbes. If any are seen, the blood is cultured (streaked) onto a variety of different agars designed to capture growth of any potential aerobics, anaerobes, or microaerophilic organisms to isolate for individual microbial colonies for full identification and specification and susceptibility testing (for antimicrobials). It is critical for bloodstream infections, also known as "bacteremia", be identified and treated as soon as possible for the best prognosis, so rapid methods of testing, including PCR and MALDI-TOF, are now available to save time.
A false positive can occur if the blood culture bottle is contaminated with skin flora. A false negative can occur if the patient started antimicrobials before the blood culture bottles were drawn, or if not enough blood was drawn so the blood-to-broth ratio is too low. Blood culture bottles are placed in an incubator, as seen above, which maintains them at a specific temperature and gently shakes them for up to 7 days (longer for fungal and AFB bottles). There are carbon dioxide sensors on the bottom that sense gases produced by microbes during the fermentation process. There is sterile broth with nutrients inside the bottles.
If the machine alarms, the blood culture bottle is removed and a Gram-stain is performed (initial) to look for microbes. If any are seen, the blood is cultured (streaked) onto a variety of different agars designed to capture growth of any potential aerobics, anaerobes, or microaerophilic organisms to isolate for individual microbial colonies for full identification and specification and susceptibility testing (for antimicrobials). It is critical for bloodstream infections, also known as "bacteremia", be identified and treated as soon as possible for the best prognosis, so rapid methods of testing, including PCR and MALDI-TOF, are now available to save time.
true blood infections versus common blood culture contaminants:
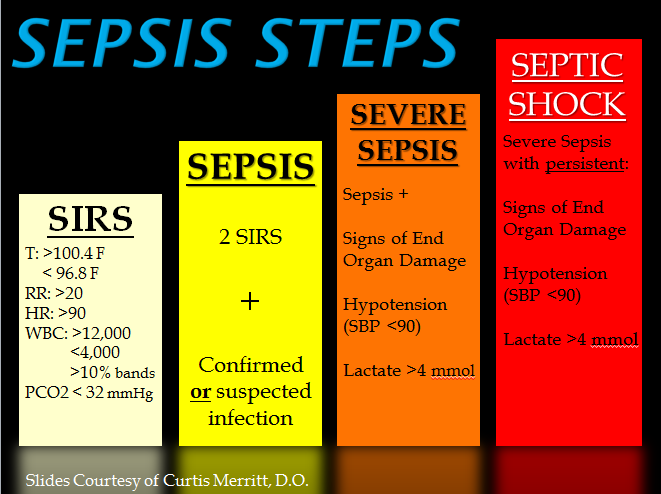
Blood is normally sterile, containing no microorganisms. If bacteria enter the blood, it is referred to as bacteremia, which can progress to sepsis. If fungi enter the blood, it is known as fungemia. If parasites enter the blood, it is known as parasitemia. If viruses enter the blood, it is known as viremia. Bacteria can enter the bloodstream through cuts, wounds, punctures, cellulitis, urinary tract infections, catheters, pneumonia, ulcers, or even intravenous lines (IV lines). Persistent bacteremia or bacterial endocarditis affecting the heart can be very serious. Patients with underlying issues with their immune systems are at higher risk of infection. If the bacteria spreads, it can lead to varying degrees of sepsis, which can be life-threatening and is very serious. Sepsis results from systemic inflammation to the presence of bacteria. Sepsis can cause organ damage, or even death, if it is not treated as soon as possible. The presence of a fever and leukocytosis, particularly elevated neutrophils, are often the first signs of sepsis. Sepsis can cause the blood pressure to fall, resulting in hypotension and shock. Risk factors for all include:
The most common causes of TRUE bacteremia and fungemia include:
Blood that is drawn incorrectly or improperly or improper preparation of the patient prior to the draw can result in contamination of the blood culture bottles with normal skin microflora. The most commonly found contaminants include:
- Immunocompromised
- HIV/AIDS
- Diabetes mellitus
- Elderly
- Chronic hemodialysis
- Organ transplant
- Stem cell transplant
- Liver failure
- Spleen removal
- Treatment with steroid medications (autoimmune disease treatment, etc...)
The most common causes of TRUE bacteremia and fungemia include:
- Staphylococcus aureus (the most common cause)
- IV Catheters
- Urinary Catheters
- Skin Ulcerations
- Wounds
- Surgical Procedures
- Respiratory Infections
- MRSA
- Escherichia coli
- Most often secondary to urinary tract infections
- Enterobacteriaceae family
- Enterococcus
- IV catheters
- Urinary catheters
- Surgical Wounds
- Pseudomonas aeruginosa
- Risk factor: ICU
- Enterobacter spp
- Risk factor: ICU
- Salmonella spp
- Gastroenteritis
- Urinary tract infection secondary to gastroenteritis
- Seeds into bloodstream
- Group A Streptococcus
- Group B Streptococcus
- Streptococcus bovis (in patients with colon cancer)
- Candida albicans (yeast)
Blood that is drawn incorrectly or improperly or improper preparation of the patient prior to the draw can result in contamination of the blood culture bottles with normal skin microflora. The most commonly found contaminants include:
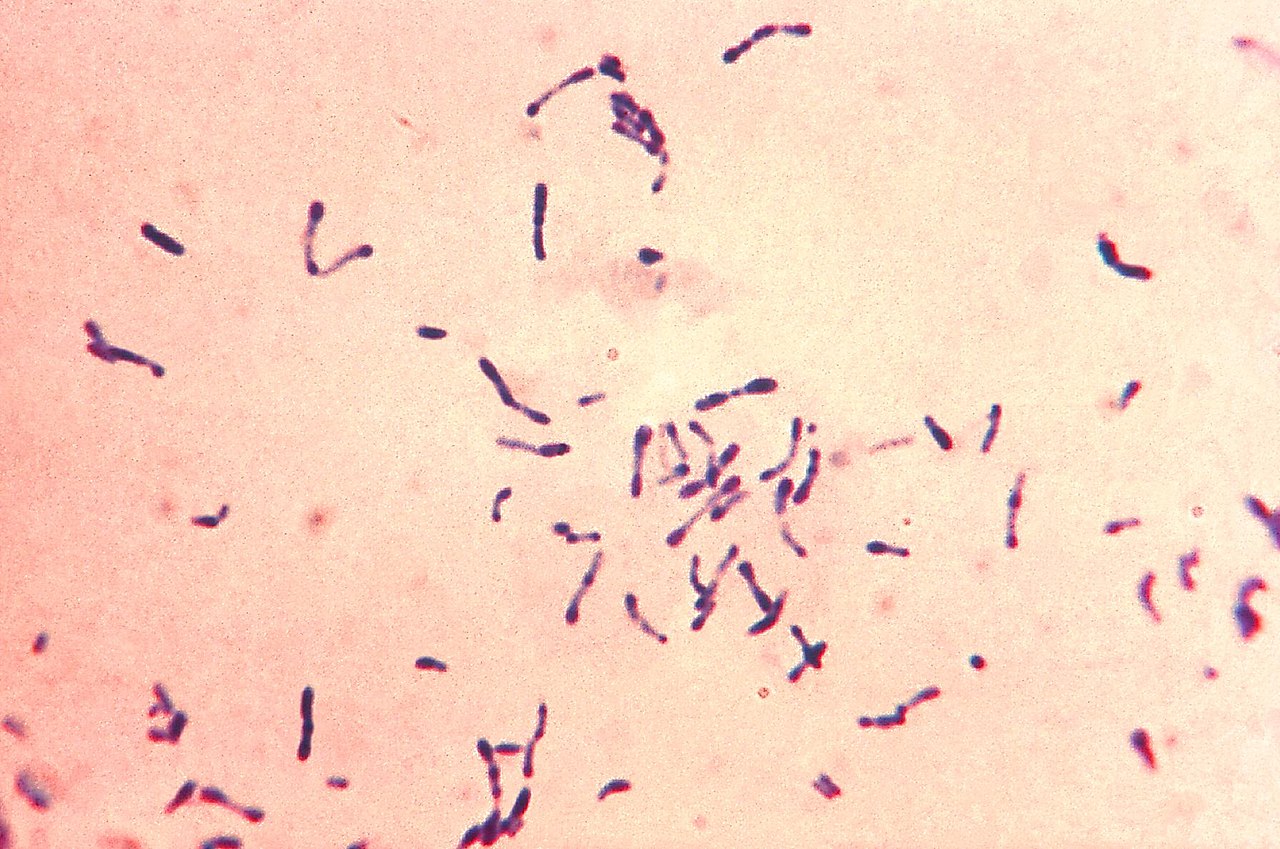
- Corynebacterium spp
- Gram-positive, coryneform, palisades bacilli
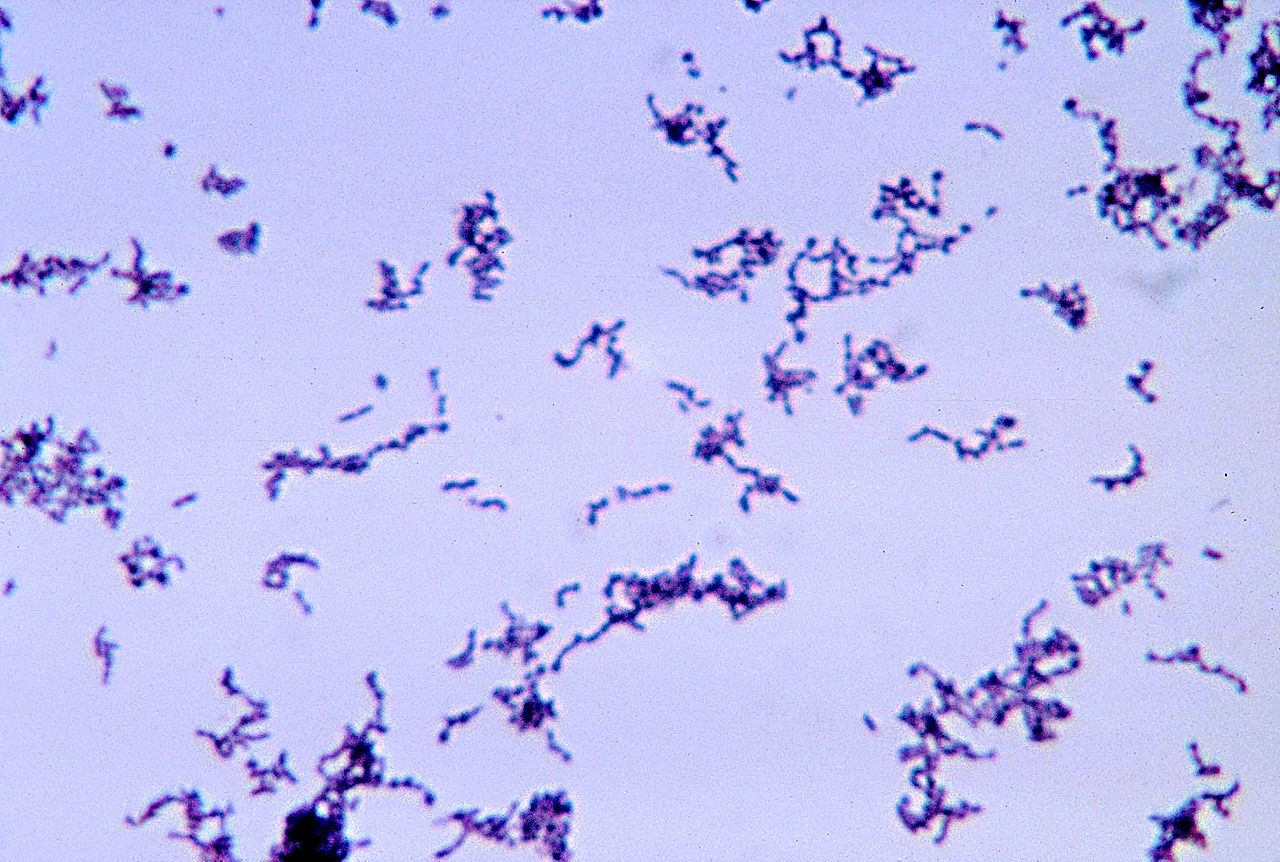
- Cutibacterium acnes (Propionibacterium)
- Gram-positive bacilli
- Staphylococcus epidermidis
- Gram-positive cocci in clusters
- Coagulase-negative Staphylococcus
- NOTE: The Staphylococcus spp listed above CAN and do cause some significant infections, but if only 1 bottle or 1 of 2 or more sets of bottles contains them, chances are it is contamination with the normal skin microflora
- Gram-positive cocci in clusters